*NURSING > CASE STUDY > NRNP 6540 Case Study 1: CC: Mrs. L.,| NRNP 6540 Case Study 1: CC: Mrs. L.,(answered) complete guide, (All)
NRNP 6540 Case Study 1: CC: Mrs. L.,| NRNP 6540 Case Study 1: CC: Mrs. L.,(answered) complete guide, to help you ace on your study (latest summer 2021/2022)
Document Content and Description Below
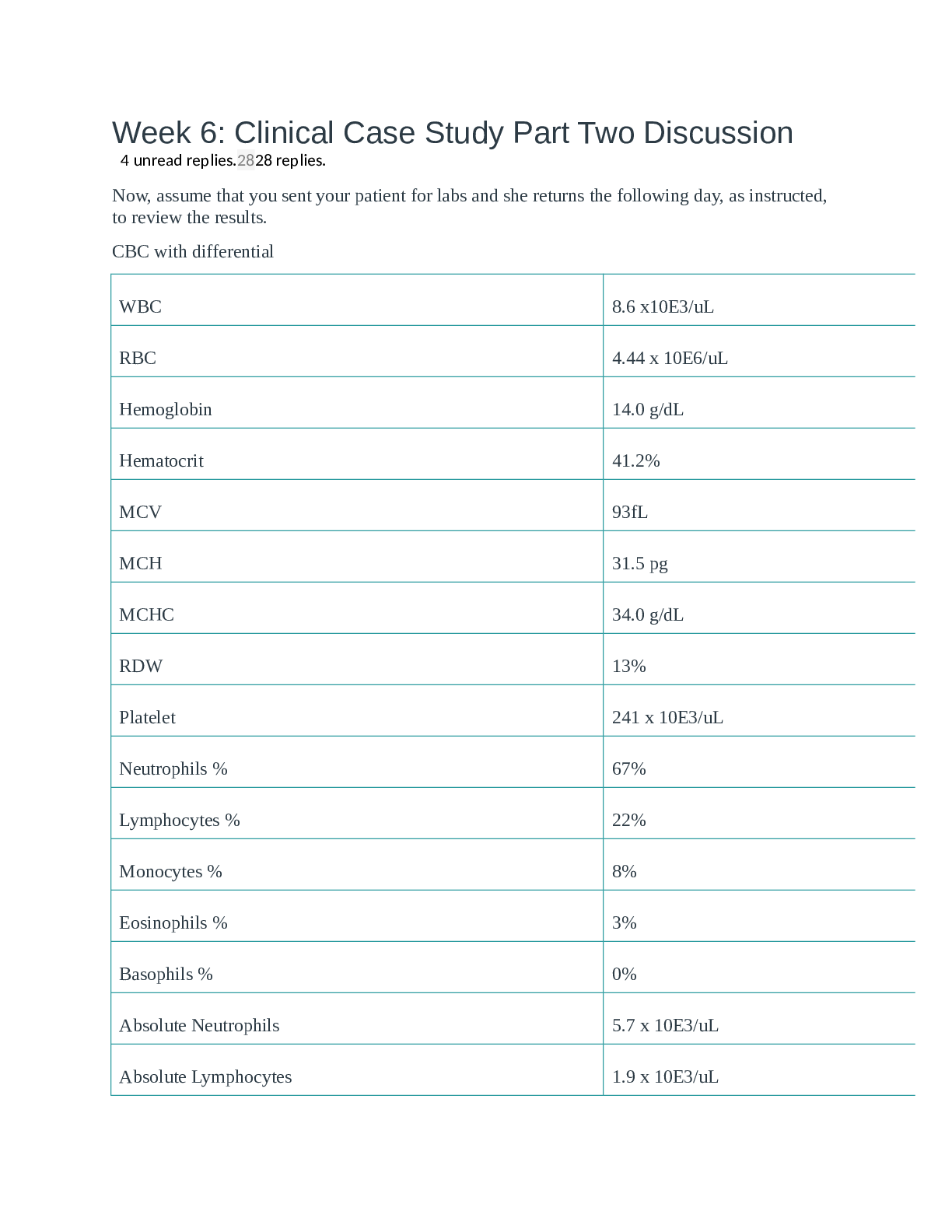
(Answered) NRNP 6540 Case Study 1: Question CC: Mrs. L., a 68-year-old woman, presents to your office today with a complaint of feeling tired all the time and now, more recently, feeling weak and ... like "I can't catch my breath sometimes." HPI: She has been healthy except for high cholesterol, managed by Lipitor. Her husband died 9 months ago, and she has attributed her fatigue to dealing with his death but realizes that she is feeling worse and not better as time passes. No known drug allergies. Medications: Takes only Lipitor. Past surgical history: Appendectomy in childhood; hysterectomy for uterine myoma 10 years ago. No significant medical history. Has two daughters living nearby. Blood pressure (BP) 106/70 mm Hg, heart rate (HR) 98 beats/min and regular, respiratory rate 18 breaths/min and afebrile, body mass index (BMI) 22 (10-pound weight loss since death of husband). Slender, quiet-spoken older woman appearing tired. PE: Conjunctiva pale, mucous membranes moist. No lymphadenopathy of neck or femoral area. Heart tachyarrhythmia with regular rate, soft midsystolic murmur. Chest (CTA), good air movement. Abdomen soft, bowel sounds × 4. Diagnostics: Urine dipstick negative. The results of a colonoscopy show a neoplasm in the colon. 1. What additional subjective data should we look for? 2. What additional objective data will be assessing for? 3. What medical history to obtain from the patient? List at least three. 4. What tests to order? Describe at least four lab tests. 5. What are the differential diagnoses to consider? Describe two. 6. What is the plan of care? List at least two diagnostic tests to be ordered to evaluate the cause of her condition. This study source was downloaded by 100000831988016 from CourseHero.com on 04-05-2022 13:56:12 GMT -05:00 https://www.coursehero.com/file/83267355/Answered-Copypdf/ Answered by Expert Tutors 1. The additional subjective data we should look for include - • How long have she had the symptoms? • Are her symptoms getting worse? • Do she smoke or use other types of tobacco? 2. Additional objective data will be assessing for - • Persistent change in her bowel habits, including diarrhea or constipation or a change in the consistency of her stool • Rectal bleeding or blood in her stool • Persistent abdominal discomfort, such as cramps, gas or pain 3. Medical history(importantly family ) to obtain from the patient is - • Making sure to document her mother's side of the family and her father's side of the family with any significant findings • Documenting which relatives have had cancer, the type(s) of cancer they have had, and the ages at which they were diagnose 4. Tests to order - 1. Colonoscopy (best), look for synchronous lesions 2. Alternative: air contrast barium enema ("apple core" lesion) + sigmoidoscopy 3. Metastatic workup: CXR, abdominal CT/ultrasound 5.Differential diagnoses to consideR 1. IBS 2. Ulcerative colitiss3. 3.Chrons disease 6. Plan of careThis study source was downloaded by 1000008319880 [Show More]
Last updated: 1 year ago
Preview 1 out of 6 pages

Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
Apr 05, 2022
Number of pages
6
Written in
Additional information
This document has been written for:
Uploaded
Apr 05, 2022
Downloads
0
Views
65
















.png)

.png)
.png)





 (1).png)





