Education > QUESTIONS & ANSWERS > NURS 612 exam 3CA: All Answers Explained By Instructor (All)
NURS 612 exam 3CA: All Answers Explained By Instructor
Document Content and Description Below
NURS 612 exam 3CA: All Answers Explained By Instructor • Conversion of fat-soluble wastes to water-soluble material for renal excretion is a function of the a. spleen. b. kidney. c. ... liver. d. pancreas. e. gallbladder. ANS: C The liver is responsible for converting fat-soluble waste to water-soluble materials so the kidneys can excrete them as well as convert ammonia to urea. REF: p. 373 • Contraction of the gallbladder propels bile into the a. stomach. b. duodenum. c. jejunum. d. ileum. e. cecum. ANS: B With contraction of the gallbladder, bile is excreted into the duodenum. REF: p. 373 • Which abdominal organs also produce hormones and function as endocrine glands? a. Kidney and liver b. Liver and gallbladder c. Stomach and spleen d. Gallbladder and pancreas e. Pancreas and kidney ANS: E The pancreas produces pancreatic juices as well as insulin and glucagon; the kidneys produce urine as well as the hormones rennin and erythropoietin. REF: p. 373 • Which organ(s) are located in the retroperitoneal space? a. Kidneys b. Lungs c. Spleen d. Gallbladder e. Liver ANS: A The kidneys are located in the retroperitoneal space, lying behind the abdominal cavity and beside the abdominal aorta. REF: p. 373 • Mrs. G is 7 months’ pregnant and states that she has developed a problem with constipation. She eats a well-balanced diet and is usually regular. You should explain that constipation is common during pregnancy because of changes in the colorectal areas, such as a. decreased movement through the colon and increased water absorption from stool. b. increased movement through the colon and increased salt taken from foods. c. looser anal sphincter and less nutrients taken from foods. d. tighter anal sphincter and less iron eliminated in the stool. e. increased absorption of nutrients and water in the colon. ANS: A Constipation and flatus are more common during pregnancy because the colon is displaced, peristalsis is decreased, and water absorption is increased. The colon does not absorb nutrients, and a tighter sphincter tone is not related to pregnancy. REF: p. 374 • The most pronounced functional change of the gastrointestinal (GI) tract in older adults is a. decreased hydrochloric acid production. b. increased motility. c. decreased bile absorption. d. decreased motility. e. increased saliva secretion. ANS: D A decrease in motility of the gastrointestinal (GI) tract is the most pronounced GI change in older adults. REF: p. 375 • The family history of a patient with diarrhea and abdominal pain should include inquiry about cystic fibrosis because it a. only affects the GI tract. b. is one cause of malabsorption syndrome. c. is a curable condition with medical intervention. d. is the most frequent cause of diarrhea in general practice. e. is a common genetic disorder. ANS: B Cystic fibrosis is an uncommon, chronic genetic disorder affecting multiple systems. In the gastrointestinal tract, it causes malabsorption syndrome because of pancreatic lipase deficiency. Steatorrhea and abdominal pain from increased gas production are frequent concerns. REF: p. 377 • Infants born weighing less than 1500 g are at higher risk for a. hepatitis A. b. necrotizing enterocolitis. c. urinary urgency. d. cystic fibrosis. e. pancreatitis. ANS: B Necrotizing enterocolitis is a gastrointestinal disease that mostly affects premature infants; it involves infection and inflammation that causes destruction of the bowel, and it becomes more apparent after feedings. Low birth weight does not relate to the development of hepatitis A, urinary urgency, cystic fibrosis, or pancreatitis. REF: p. 377 • Inspection of the abdomen should begin with the patient supine and the examiner a. seated on the patient’s right side. b. standing at the foot of the table. c. standing at the patient’s left. d. walking around the table. e. seated on the patient’s left side. ANS: A This preferred initial position allows tangential viewing of the abdomen for improved assessment of abdominal contour. REF: p. 377 • Before performing an abdominal examination, the examiner should a. ascertain the patient’s HIV status. b. have the patient empty his or her bladder. c. don double gloves. d. completely disrobe the patient. e. uncover only the painful areas of the abdomen. ANS: B The patient should empty the bladder to ensure an accurate examination of organs as well as to provide comfort for the patient. REF: p. 377 • Which structure is located in the hypogastric region of the abdomen? a. Bladder b. Cecum c. Gallbladder d. Stomach e. Liver ANS: A The hypogastric (pubic) area contains the ileum, the bladder, and the pregnant uterus. REF: p. 379 • Murphy's Sign pain on inspiration .Examiner's fingers are placed on the RUQ at the gallbladder, a finding associated with acute cholecystitis • When examining a patient with tense abdominal musculature, a helpful technique is to have the patient a. hold his or her breath. b. sit upright. c. flex his or her knees. d. raise his or her head off the pillow. e. fully extend the legs. ANS: C To help relax the abdominal musculature, it is helpful to place a small pillow under the patient’s head and under slightly flexed knees. The other choices increase muscle flexion. REF: p. 383 • You ask the patient to raise the head and shoulders while lying in a supine position. A midline abdominal ridge rises. You chart this observation as a(n) a. small inguinal hernia. b. large epigastric hernia. c. abdominal lipoma. d. diastasis recti. e. incisional hernia. ANS: D A diastasis recti occurs when abdominal contents bulge between two abdominal muscles to form a midline ridge as the head is lifted. It has little clinical significance and most often occurs in repeated pregnancies and obesity. REF: p. 395 • What condition is associated with striae that remain purplish? a. Cushing disease b. Diastasis recti c. Liver cirrhosis d. Recent pregnancy e. Intraabdominal bleeding ANS: A Striae from pregnancy or obesity begin as a pink or purple color then turn silvery white; striae associated with Cushing disease stay purplish. REF: p. 379 • Valgus sign Outward angulation of distal segment of bone or joint- medial meniscus or medial collateral ligament damage (ex: football injury) • Visible intestinal peristalsis may indicate a. normal digestion. b. intestinal obstruction. c. increased pulse pressure of aorta. d. aortic aneurysm. e. paralytic ileus. ANS: B Peristalsis is not usually visible and when detected may indicate an intestinal obstruction. REF: p. 381 • After thorough inspection of the abdomen, the next assessment step is to a. percuss. b. palpate nonpainful areas. c. auscultate. d. perform a rectal examination. e. palpate painful areas. ANS: C Assessment of the abdomen begins with inspection followed by auscultation. This break from the usual system examination sequence is because palpation and percussion can alter the frequency as well as the intensity of bowel sounds. Therefore, auscultation is done first. REF: p. 381 • Auscultation of borborygmi is associated with a. gastroenteritis. b. peritonitis. c. satiety. d. paralytic ileus. e. stenotic arteries. ANS: A Borborygmi are prolonged loud gurgles that occur with gastroenteritis, early intestinal obstruction, or hunger. Peritonitis and paralytic ileus result in hypoactive bowel sounds. Food satiety does not stimulate growling sounds as hunger does. Vascular bruits are not associated with borborygmi. REF: p. 381 • Peritonitis often produces bowel sounds that are a. decreased. b. increased. c. high pitched. d. absent. e. accentuated. ANS: A Decreased bowel sounds occur with peritonitis and paralytic ileus. REF: p. 381 • A patient is complaining of abdominal pain, nausea with vomiting, malaise, and a low-grade fever attributed to eating some “bad food” 4 hours ago. The abdomen is soft and rounded, with hypoactive bowel sounds after 5 minutes of auscultation to each quadrant. Which assessment finding is inconsistent with gastroenteritis? a. Malaise b. Low-grade fever c. Hypoactive bowel sounds d. Soft, rounded abdomen e. Abdominal pain ANS: C Gastroenteritis is more consistent with findings of crampy abdominal pain, borborygmi, nausea and vomiting, diarrhea, fever, and no abdominal distention. Hypoactive bowel sounds are not expected with gastroenteritis. A firm, distended abdomen suggests an obstruction. REF: p. 381 • An examiner can recognize a friction rub in the liver by a sound that is a. clicking, gurgling, and irregular. b. high pitched and associated with respirations. c. loud, prolonged, and gurgling. d. soft, low-pitched, and continuous. e. low pitched, tinkling, and unrelated to respirations. ANS: B An abdominal friction rub is rare and can be identified when high-pitched sounds are auscultated in association with respirations. REF: p. 381 • To correctly document absent bowel sounds, one must listen continuously for a. 30 seconds. b. 1 minute. c. 3 minutes. d. 5 minutes. e. 10 minutes. ANS: D Absent bowel sounds are confirmed after listening to each quadrant for 5 minutes. REF: p. 381 • Percussion at the right midclavicular line, below the umbilicus, and continuing upward is the correct technique for locating the a. descending aorta. b. lower liver border. c. medial border of the spleen. d. upper right kidney ridge. e. stomach. ANS: B Percussing along the right midclavicular line upward from the umbilicus determines the lower border of the liver. A liver border more than 2 to 3 cm signifies hepatomegaly. REF: p. 381 • When auscultating the abdomen, which finding would indicate collateral circulation between the portal and systemic venous systems? a. Arterial bruit b. Gastric rumbling c. Renal hyperresonance d. Borborygmi e. Venous hum ANS: E Venous hum is associated with blood flow in venous collaterals found in portal hypertension. Aortic bruit occurs during systole, and a venous hum is a continuous sound and softer than a bruit. The other choices are not vascular sounds. REF: p. 381 • Percussion of the abdomen begins with establishing a. liver dullness. b. spleen dullness. c. gastric bubble tympany. d. overall dullness and tympany in all quadrants. e. bladder fullness. ANS: D Percussion begins with a general establishment over all quadrants for areas of dullness and tympany and then proceeds to specific target organs. REF: p. 381 • To assess for liver enlargement in an obese person, you should a. use the hook method. b. test for cutaneous hypersensitivity. c. auscultate using the scratch technique. d. attempt palpation during deep exhalation. e. have the patient lean over at the waist. ANS: C If the abdomen is obese or distended or if the abdominal muscles are tight, you should plan on auscultating the liver using the scratch method to estimate the lower border of the liver. Cutaneous hypersensitivity is a sign of peritonitis and does not contribute to determining liver size. REF: p. 386 • An umbilical assessment in the newborn that is of concern is a. a thick cord. b. an umbilical hernia. c. one umbilical artery and two veins. d. pulsations superior to the umbilicus. e. visible nondistended superficial veins. ANS: C What is expected is two arteries and one vein. A single umbilical artery indicates the possibility of congenital anomalies. A thick cord suggests a well-nourished fetus, an umbilical hernia will generally spontaneously close by 2 years, and pulsations to the abdomen in the epigastric area are common. Nondistended superficial veins are usually visible in thin infants. REF: p. 394 • Failure to pass a meconium stool in the first 24 hours after birth along with abdominal distention is often the first sign of a. Meckel diverticulum. b. cystic fibrosis. c. biliary atresia. d. hydramnios. e. Wilms tumor. ANS: B Meconium ileus is often the first manifestation of cystic fibrosis or Hirschsprung disease. REF: p. 411 • When palpating the aorta, a prominent lateral pulsation suggests a. aortic aneurysm. b. normal pulsation. c. renal artery fistula. d. vena cava varicosity. e. coarctation. ANS: A Anterior pulsations of the aorta are within normal limits; lateral pulsations suggest an aortic aneurysm. REF: p. 388 • A patient presents with symptoms that lead you to suspect acute appendicitis. Which assessment finding is least likely to be associated with this condition early in its course? a. Positive psoas sign b. Positive McBurney sign c. History of periumbilical pain d. Rebound tenderness e. Obturator muscle test ANS: E Psoas sign, McBurney point pain, rebound tenderness, and periumbilical pain that migrates to the right lower quadrant are signs of appendicitis. Conditions that cause irritation of the obturator muscle are late findings usually associated with a ruptured appendix or pelvic abscess. REF: p. 393 • When using the bimanual technique for palpating the abdomen, you should a. push down with the bottom hand and the other atop. b. push down with the top hand and the other atop. c. place hands side by side and push equally. d. place one hand anteriorly and the other posteriorly squeezing the hands together. e. make a fist with the top hand and strike the bottom hand. ANS: B The bimanual technique uses one hand on top of the other with the top hand pushing down while the bottom hand against the abdomen is used for sensing. REF: p. 394 • A 23-year-old man comes to the urgent care clinic with intense left flank and lower left quadrant pain. One patient response to history of present illness questions that further supports a tentative diagnosis of renal calculi is a. “My urine has been bright yellow.” b. “I have had fever and chills for 2 days.” c. “I also have a headache and neck ache.” d. “My left testicle and shoulder hurt as well.” e. “I have had flatulence and foul-smelling urine.” ANS: D Renal calculi present with hematuria, intermittent flank pain that radiates to the groin and genitals, and a positive Kehr sign (pain radiating to the left shoulder). REF: p. 391 • Flatulence, diarrhea, dysuria, and tenderness with abdominal palpation are findings most associated with a. peptic ulcer disease. b. pancreatitis. c. ruptured ovarian cyst. d. splenic rupture. e. diverticulitis. ANS: E No choice other than diverticulitis has all of these presenting symptoms. REF: p. 390 • A 45-year-old man relates a several-week history of severe intermittent abdominal burning sensations. He relates that the pain is relieved with small amounts of food. Before starting the physical examination, you review his laboratory work, anticipating a(n) a. elevated white blood cell count. b. decreased potassium level. c. positive Helicobacter pylori result. d. increased urine specific gravity. e. folate deficiency. ANS: C The patient’s presenting symptoms suggest peptic ulcer disease. The supporting laboratory finding is the presence of H. pylori. REF: p. 401 • A 51-year-old woman calls with concerns of weight loss and constipation. She reports enlarged hemorrhoids and rectal bleeding. You advise her to a. use topical over-the-counter hemorrhoid treatment for 1 week. b. exercise and eat more fiber. c. come to the laboratory for a stool guaiac test. d. eat six small meals a day. e. go to the emergency department for a barium enema. ANS: C Blood in the stools is an abnormal finding that should never be ignored even if it can be explained by conditions other than colon cancer. She should have her stool checked for blood now as well as annually because she is older than 50 years. REF: p. 404 • Patients presenting with ascites, jaundice, cutaneous spider veins, and nonpalpable liver exhibit signs of a. cholecystitis. b. pancreatitis. c. inflammatory bowel disease. d. diverticulitis. e. cirrhosis. ANS: E Jaundice is a result of excessive bilirubin that can result from cholecystitis, pancreatitis, or liver problems. Cirrhosis presents with additional symptoms of ascites, cutaneous spider veins, and a nonpalpable liver as scarring progresses. REF: p. 404 • A patient presents to the emergency department after a motor vehicle accident. The patient sustained blunt trauma to the abdomen and complains of pain in the upper left quadrant that radiates to the left shoulder. What organ is most likely injured? a. Gallbladder b. Liver c. Spleen d. Stomach e. Colon ANS: C Spleen laceration or rupture is always suspected with abdominal injury because of its anatomic location. The patient’s presenting symptoms confirm this suspicion. REF: p. 407 • Costovertebral angle tenderness should be assessed whenever you suspect the patient may have a. cholecystitis. b. pancreatitis. c. pyelonephritis. d. ulcerative colitis. e. intussusception. ANS: C Pyelonephritis is characterized by flank pain and costovertebral angle tenderness. REF: p. 408 • Imaging studies reveal that a patient has dilation of the renal pelvis from an obstruction in the ureter. What condition will be documented in this patient’s health record? a. Glomerulonephritis b. Hydronephrosis c. Pyelonephritis d. Renal abscess e. Renal artery emboli ANS: B Hydronephrosis is the dilation of the renal pelvis from back pressure of urine that cannot flow past an obstruction in the ureter. REF: p. 408 • The most common congenital anomaly of the gastrointestinal tract is a. biliary atresia. b. meconium ileus. c. intussusception. d. Meckel diverticulum. e. pyloric stenosis. ANS: D Meckel diverticulum is the most common congenital anomaly of the gastrointestinal tract. REF: p. 412 • Baby Joe is 6 months old. He has abdominal distention and vomiting and is inconsolable. A sausage-shaped mass is palpable in his right upper quadrant. Joe’s lower quadrant feels empty, and a positive Dance sign is noted in his record. Which one of the following conditions is consistent with Baby Joe’s symptoms? a. Intussusception b. Kidney stones c. Meconium ileus d. Pyloric stenosis e. Necrotizing enterocolitis ANS: A Intussusception refers to the prolapse of one segment of the intestine into another causing intestinal obstruction. Whereas a sausage-shaped mass may be palpated in the right or left upper quadrant, the lower quadrant feels empty (positive Dance sign); it commonly occurs between 3 and 12 months of age. REF: p. 410 • A mother brings her 2-year-old child for you to assess. The mother feels a lump whenever she fastens the child’s diaper. Nephroblastoma is likely for this child when your physical examination of the abdomen reveals a(n) a. fixed mass palpated in the hypogastric area. b. tender, midline abdominal mass. c. olive-sized mass of the right upper quadrant. d. nontender, slightly moveable, flank mass. e. sausage-shaped mass in the left upper quadrant. ANS: D A Wilms tumor (nephroblastoma) is the most common intraabdominal tumor of childhood. It presents with hypertension; fever; malaise; and a firm, nontender mass deep within the flank that is only slightly movable and is usually unilateral. REF: p. 413 • A 1-month-old boy has been vomiting for 2 weeks. How is this symptom of gastroesophageal reflux disease (GERD) and pyloric stenosis further differentiated in this child’s assessment? a. Vomiting becomes projectile with GERD. b. The infant has regurgitation with pyloric stenosis. c. An olive-sized mass of the right upper quadrant (RUQ) occurs with GERD. d. Normal stools are expected with pyloric stenosis. e. The fontanel becomes sunken with pyloric stenosis. ANS: B With pyloric stenosis, vomiting becomes projectile, and a small olive-sized mass is palpable in the RUQ; the infant is usually hungry again soon after vomiting, and because little or no food is reaching the intestines, the infant has fewer, smaller stools. The child fails to thrive and has signs of dehydration. These signs are not associated with GERD. Regurgitation can be present with either disease. REF: p. 410 • Urinary incontinence that occurs from the inability to hold urine when the stimulus to urinate is perceived is called _____ incontinence. a. paralytic b. urge c. overflow d. functional e. stress ANS: B Urge incontinence is the inability to delay urination when the urge to void occurs. REF: p. 415 • In older adults, overflow fecal incontinence is commonly caused by a. malabsorption. b. parasitic diarrhea. c. Meckel diverticulum. d. fistula formation. e. fecal impaction. ANS: E Constipation with overflow occurs when the rectum contains hard stool and soft feces above leak around the mass of stool. REF: p. 415 • Fluid that lubricates articular cavities is called a. blood. b. synovial fluid. c. mucus. d. cerumen. e. marrow. ANS: B Articular cavities are lined with synovial membrane, which secretes synovial fluid that provides lubrication for the joint to move. REF: p. 501 • Bones around a joint are held together by a. synovial membranes. b. ligaments. c. muscles. d. cartilage. e. tendons. ANS: B Bones are held together within a joint by ligaments. Synovial membranes secrete synovial fluids, which provide lubrication to the joints. Tendons attach muscle to bone, bones are not held together by muscles, and cartilage forms most of the joints in the adult skeleton and merely acts as a shock absorber. REF: p. 501 • Bones are attached to muscles by a. synovial membranes. b. ligaments. c. muscles. d. cartilage. e. tendons. ANS: E Tendons attach muscle to bone. Synovial membranes secrete synovial fluids, which provide lubrication to the joints. Ligaments attach bone to bone. Muscles are not bound together by other muscles, and cartilage helps in the production of new bone and acts as an insulator for bones in joints. REF: p. 501 • The elbow joint that allows for flexion and extension in one plane represents a type of _____ joint. a. articulated b. ball and socket c. hinge d. pivot condyloid e. saddle ANS: C A hinge joint allows for flexion and extension in one plane. A condyloid joint allows flexion and extension in two planes. A ball and socket joint allows movement in all planes. An articulated joint means simply that the joint allows movement. A saddle joint allows motion in two planes at right angles to each other but no axial rotation. REF: p. 505 • Spinal vertebrae are separated from each other by a. bursae. b. tendons. c. disks d. ligaments. e. synovial fluid. ANS: C Except for sacral vertebrae, the spinal vertebrae are separated from one another by fibrocartilaginous disks. REF: p. 505 • The glenohumeral joint is the other name for the a. elbow. b. hip. c. wrist. d. scapula. e. shoulder. ANS: E The shoulder joint, also called the glenohumeral joint, consists of the union between the humerus and the scapula. REF: p. 505 • The joint where the humerus, radius, and ulna articulate is the a. wrist. b. elbow. c. shoulder. d. sternum. e. clavicle. ANS: B The elbow is the site where the humerus, radius, and ulna meet. The shoulder is made up of the humerus and scapula. The wrist is made up of the radius and the carpal bones of the hand. The sternum connects to the clavicles and ribs. The clavicle connects to the scapula but not the humerus. REF: p. 505 • The articulation of the radius and carpal bones is the a. wrist. b. elbow. c. shoulder. d. clavicle. e. digits. ANS: A The joint composing the radius and carpal bones is called the wrist. REF: p. 505 • The cruciate ligaments within the knee provide for a. anterior and posterior stability. b. medial and lateral stability. c. movement on one plane. d. pivoting and rotation. e. shock absorption. ANS: A The cruciate ligaments within the knee are positioned so as to provide anterior and posterior stability. The collateral ligaments maintain medial and lateral stability. The knee joint is a hinge joint that allows movement in one plane. Cartilage is the structure that provides shock absorption. REF: p. 507 • Medial and lateral surfaces of the tibiotalar joint are protected by a. bursae. b. tendons. c. muscles. d. ligaments. e. synovial fluid. ANS: D The ankle joint, or tibiotalar joint, is protected by ligaments on the medial and lateral sides. Bursae, tendons, muscles, and synovial fluid do not offer stabilization protection to the ankle. REF: p. 507 • The suprapatellar bursa separates the patella, quadriceps tendon, and muscle from the a. talus. b. fibula. c. femur. d. pelvis. e. tibia. ANS: C The suprapatellar bursa separates the knee, the quadriceps, and muscle from the femur. REF: p. 507 • The tibia, fibula, and talus articulate to form the a. ankle. b. knee. c. hip. d. pelvis. e. forefoot. ANS: A The tibia, fibula, and talus, or heel, join to form the ankle. REF: p. 507 • Long bones in children have growth plates known as a. epiphyses. b. epicondyles. c. synovium. d. fossae. e. diastasis. ANS: A Epiphyses are the growth plates found in long bones in children. REF: p. 508 • Ligaments are stronger than bone until a. birth. b. infancy. c. adolescence. d. middle adulthood. e. old age. ANS: C Ligaments are stronger than bone during birth and infancy. It is not until adolescence that bone becomes stronger. REF: p. 508 • Injuries to long bones and joints are more likely to result in fractures than in sprains until a. preschool age. b. school age. c. adolescence. d. early adulthood. e. middle adulthood. ANS: C Fractures to long bones and joints are more common during growth years. During childhood and early adolescence, the epiphyseal growth plates are more easily injured than are the tougher ligaments. Growth is completed with the closure of the epiphyseal growth plates at about 20 years of age. REF: p. 508 • The elasticity of pelvic ligaments and softening of cartilage in a pregnant woman are caused by a. decreased mineral deposition. b. increased hormone secretion. c. uterine enlargement. d. gait changes. e. increased mineral resorption. ANS: B Increased hormone secretion during pregnancy is responsible for the elasticity of pelvic ligaments and softening of the cartilage. These changes help accommodate the growing fetus. REF: p. 508 • Skeletal changes in older adults are the result of a. increased bone deposition. b. increased bone resorption. c. tendons becoming more elastic. d. decreased bone deposition. e. decreased bone resorption. ANS: B As a person ages, the skeletal system undergoes several changes. One of the dramatic changes in skeletal equilibrium is that bone resorption dominates bone deposition. Tendons become less elastic in older adults. REF: p. 508 • The usual number of vertebrae is a. 23. b. 24. c. 25. d. 26. e. 27. ANS: B The number of vertebrae that is most common is 24; as few as 11% of persons have 23, and almost 5% have 26. REF: p. 504 • + Romberg Sign Loss of balance that occurs when closing the eyes , occurs with: ◦ cerebellar ataxia ◦ loss of proprioception ◦ loss of vestibuar function • The family history for a patient with joint pain should include information about siblings with a. trauma to the skeletal system. b. chronic atopic dermatitis. c. genetic disorders. d. obesity. e. poor physical conditioning. ANS: C An important history to obtain for a patient with joint pain would be family history of genetic disorders such as osteogenesis imperfecta, dwarfing syndrome, rickets, hypophosphatemia, or hypercalciuria. REF: p. 509 • Risk factors for sports-related injuries include a. competing in colder climates. b. previous fractures. c. history of recent weight loss. d. failure to warm up before activity. e. light body frame. ANS: D Failure to warm up before exercise is one risk factor for sports-related injuries. Climate, previous fractures, and weight loss are not as strong risk factors for sports-related injuries. A light body frame is a risk factor for osteoporosis, not sports-related injuries. REF: p. 539 • Light skin and thin body habitus are risk factors for a. rheumatoid arthritis. b. osteoarthritis. c. congenital bony defects. d. osteoporosis. e. sports-related injuries. ANS: D People with light skin and a thin body frame are at greater risk for developing osteoporosis. Rheumatoid arthritis, osteoarthritis, bony defects, and sports-related injuries are not found to have a correlation with light skin and a small frame. REF: p. 510 • Inquiry about nocturnal muscle spasms would be most significant when taking the musculoskeletal history of a. adolescents. b. infants. c. older adults. d. middle adulthood. e. children. ANS: C History taking of older adults should consist of symptoms of nocturnal muscle spasms. Pregnant women and older adults commonly experience nocturnal leg cramps resulting from imbalances of fluids, hormones, minerals or electrolytes, or dehydration. A particular concern with the older adults is that this may be a sign of intermittent claudication. REF: p. 510 • The musculoskeletal examination should begin when a. the patient enters the examination room. b. during the collection of subjective data. c. when height is measured. d. when joint mobility is assessed. e. the remainder of the physical examination is completed. ANS: A When the patient first walks in the room, the examiner should observe the gait and posture as part of the musculoskeletal examination. REF: p. 510 • Pain, disease of the muscle, and damage to the motor neuron may all cause a. bony hypertrophy. b. muscle crepitus. c. muscle hypertrophy. d. muscle wasting. e. claudication. ANS: D Muscle wasting is a consequence of pain from injury, pathology of the muscle, and injury to the motor neuron. REF: p. 510 • An increase in muscle tone is known as a. crepitus. b. effusion. c. tenosynovitis. d. atrophy. e. spasticity. ANS: E An increase in muscle tone is referred to as spasticity. Crepitus, effusion, and tenosynovitis do not relate to muscle, and atrophy is wasting or a decrease in muscle mass. REF: p. 530 • Fasciculation occurs after injury to a muscle’s a. venous return. b. motor neuron. c. strength. d. tendon. e. fascia. ANS: B Fasciculations can often by visualized as muscle twitching or dimpling under the skin, but they usually do not generate sufficient force to move a limb. They may represent a benign condition or occur as a manifestation of motor neuron disease or peripheral nervous system diseases. REF: p. 510 • The physical assessment technique most frequently used to assess joint symmetry is a. inspection. b. palpation. c. percussion. d. the use of joint calipers. e. auscultation. ANS: A The assessment technique most commonly used to assess joint symmetry is inspection. Palpation, percussion, auscultation, and the use of joint calipers are not commonly used for this purpose. REF: p. 510 • A goniometer is used to assess a. bone maturity. b. joint proportions. c. range of motion. d. muscle strength. e. body fat. ANS: C The angle of a joint can be accurately measured using a goniometer. This is used when the joint range of motion is beyond the normal limits. Muscle strength, bone maturity, body fat, and joint proportions are not measured by a goniometer. REF: p. 511 • When palpating joints, crepitus may be caused when a. irregular bony surfaces rub together. b. supporting muscles are excessively spastic. c. joints are excessively lax. d. there is excess fluid within the synovial membrane. e. there is muscle wasting. ANS: A Crepitus is felt or heard when irregular bony surfaces rub together. Spastic muscles, muscle wasting, lax joints, and excess synovial fluid do not produce this grating sound upon palpation. REF: p. 510 • The temporomandibular joint is palpated a. under the mandible anterior to the sternocleidomastoid muscle. b. from inside the mouth. c. anterior to the tragus. d. at the mastoid process. e. above the mandible at midline. ANS: C The temporomandibular joint is palpated just anterior to the tragus of the ear; the fingertips are placed inside the joint space as the patient opens and closes the mouth. Under the mandible, above the mandible, and at the mastoid process do not describe the location of the temporomandibular joint. REF: p. 516 • Temporalis and masseter muscles are evaluated by a. having the patient frown. b. having the patient clench his or her teeth. c. asking patient to fully extend his or her neck. d. passively opening the patient’s jaw. e. having the patient shrug his or her shoulders. ANS: B Having the patient bite down and clench his or her teeth is the method to examine the strength of the temporalis and masseter muscles. Cranial nerve V is tested with this same maneuver. REF: p. 516 • The strength of the trapezius muscle is evaluated by having the patient a. clench his or her teeth during muscle palpation. b. push his or her head against the examiner’s hand. c. straighten his or her leg with examiner opposition. d. uncross his or her legs with examiner resistance. e. adduct the arm. ANS: B Having the patient apply opposite force with differing head motions, against the examiner’s hand, assesses the sternocleidomastoid and trapezius muscles. REF: p. 518 • Expected normal findings during inspection of spinal alignment include a. asymmetrical skinfolds at the neck. b. slight right-sided scapular elevation. c. convex lumbar curve. d. head positioned superiorly to the gluteal cleft. e. convex cervical curve. ANS: D Spinal alignment is considered within normal limits when the patient’s head is positioned directly over the gluteal cleft. The skin folds should be symmetrical, the scapulae are at even heights, and both the cervical and lumbar curves are concave. REF: p. 518 • A common finding in markedly obese and pregnant women is a. kyphosis. b. lordosis. c. paraphimosis. d. scoliosis. e. phimosis. ANS: B Bowing of the back, or lordosis, is more commonly found in pregnant women and obese patients because of an altered center of gravity. Kyphosis is more commonly seen in older adults, and scoliosis is more commonly seen in teenagers. Phimosis and paraphimosis are penile conditions. REF: p. 533 • When the patient flexes forward at the waist, what spinal observation would lead you to suspect scoliosis? a. A prominent lumbar hump b. A prominent cervical concave curve c. Lateral curvature of the spine d. Restricted ability to flex at the hips e. A gibbus ANS: C Scoliosis is suspected when there is a noticeable lateral curvature of the spine, or rib hump, as the patient bends forward at the waist. REF: p. 519 • When the shoulder contour is asymmetrical and one shoulder has hollows in the rounding contour, you would suspect a. a dislocated elbow. b. a fractured scapula. c. a dislocated shoulder. d. muscle wasting. e. kyphosis. ANS: C Asymmetrical contours to the shoulder with a hollowing in the socket are symptoms of a shoulder dislocation. Kyphosis is a condition of the back; muscle wasting, a dislocated elbow, and a scapula fracture do not present with these symptoms. REF: p. 514 • Ulnar deviation and boutonniere deformities are characteristic of a. winged scapula. b. osteoarthritis. c. osteoporosis. d. congenital defects. e. rheumatoid arthritis. ANS: E Deviation of the fingers toward the ulnar side and boutonniere deformities are classic symptoms of rheumatoid arthritis. Winged scapula, osteoarthritis, congenital defects, and osteoporosis do not present with these symptoms. REF: p. 513 • A finding that is indicative of osteoarthritis is a. swan neck deformities. b. Bouchard nodes. c. ganglion cysts d. Heberden nodes. e. spindle-shaped fingers. ANS: D Heberden nodes are bony overgrowths of the distal end of the fingers and are associated with osteoarthritis. When the overgrowths are concentrated in the proximal interphalangeal joint, they are known as Bouchard nodes and are associated with rheumatoid arthritis, as are swan neck deformities and spindle-shaped fingers; ganglion cysts are not associated with osteoarthritis. REF: p. 513 • A tingling sensation radiating from the wrist to the hand on striking the median nerve is a positive _____ sign. a. Phalen b. Gower c. Homan d. Tinel e. Allis ANS: D The Tinel sign is a test for carpal tunnel syndrome. A positive result is elicited when the median nerve is struck, producing a tingling sensation from the wrist toward the fingers. REF: p. 524 • Classic carpal tunnel syndrome would result in a. pain in the fourth and fifth digits. b. a negative Phalen test. c. reduced abduction of the thumb. d. palm tingling. e. a negative Tinel sign. ANS: C Median nerve compression, as in carpal tunnel syndrome, results in a positive Tinel sign, a positive Phalen sign, reduced abduction of the thumb, and sparing of palm tingling. The median half of the fourth digit and entire fifth digit are asymptomatic. REF: p. 524 • Excessive hyperextension of the knee with weight bearing may indicate a. advanced joint degeneration. b. early signs of gout. c. rotation of the Achilles tendon. d. a meniscal tear. e. weakness of the quadriceps muscle. ANS: E Genu recurvatum, which is hyperextension of the knee, is a result of quadriceps muscle weakness. Gout, joint degeneration, Achilles tendon rotation, and meniscal tears do not cause hyperextension of the knee. REF: p. 521 • Arm length is measured from the acromion process through the a. olecranon joint to carpal thumb hinge. b. olecranon process to distal ulnar prominence. c. proximal radial prominence to distal joint. d. proximal ulnar joint to middle fingertip. e. olecranon process to the second fingertip. ANS: B Total arm length is assessed by the standard measurement of the length from the shoulder (acromion process) through the elbow (olecranon process) joint to the wrist (distal ulnar prominence). REF: p. 529 • A positive straight leg raise test usually indicates a. leg length discrepancy. b. knee instability. c. lumbar nerve root irritation. d. hip bursitis. e. improperly conditioned muscles. ANS: C Lumbar nerve root irritation at the L4, L5, and S1 levels can be assessed by asking the patient to lie supine with the neck flexed and to raise one leg. If pain is felt, it is a positive straight leg raise result. The straight leg raise test does not assess leg length, knee stability, hip bursitis, or muscle condition. REF: p. 526 • The Thomas test is used to detect a. hip dislocation. b. unstable sacroiliac joints. c. knee instability. d. flexion contractures of the hip. e. asymmetry in the level of the iliac crests. ANS: D The Thomas test requires the patient to lie supine with one leg stretched out flat and the other raised and bent in toward the chest. If the patient is unable to keep the extended leg flat on the table, this is an indicator of a hip flexion contracture. The Thomas test does not assess hip dislocation, sacroiliac joints, knee instability, or asymmetry of the iliac crests. REF: p. 526 • Which one of the following techniques is used to detect a torn meniscus? a. Phalen test b. McMurray test c. Thomas test d. Trendelenburg test e. Drawer test ANS: B The McMurray test points to a meniscus tear. The Phalen test detects carpal tunnel syndrome. The drawer test detects an anterior cruciate ligament tear, the Thomas test detects hip contraction, and the Trendelenburg test detects weak hip abductor muscles. REF: p. 527 • When performing the drawer test, the examiner would place the patient in a supine position and flex the knee 45 to 90 degrees, placing the foot flat on the table, and then a. grasp and evert the foot and extend the knee. b. grasp and invert the foot and rotate the knee. c. grasp the lower leg with both hands and draw the tibia forward and then backward. d. apply varus stress with the foot planted. e. apply valgus stress after the leg is extended. ANS: C The next step is to place both hands on the lower leg with the thumbs on the ridge of the anterior tibia just distal to the tibial tuberosity. Draw the tibia forward, forcing the tibia to slide forward of the femur. Then push the tibia backward. Anterior or posterior movement of the knee greater than 5 mm in either direction is an unexpected finding. REF: p. 527 • Anterior cruciate ligament integrity is assessed via the _____ test. a. Lachman b. straight leg raise c. valgus stress d. Homan e. Thomas ANS: A The Lachman test evaluates anterior cruciate ligament integrity. The straight leg raise test assesses nerve root damage, the valgus stress test assesses instability of the lateral and medial collateral ligaments, the Homan test assesses for blood clots in the legs, and the Thomas test is used to detect flexion contractures of the hips. REF: p. 528 • During a football game, a player was struck on the lateral side of the left leg while his feet were firmly planted. He is complaining of left knee pain. To examine the left knee, you should initially perform the _____ test. a. varus stress b. valgus stress c. Apley d. Lachman e. drawer ANS: B The injury described will most likely result in a medial meniscus or medial collateral ligament damage. Your initial assessment would be to apply the valgus stress test to assess the medial meniscus. REF: p. 528 • Term infants normally resist a. ankle dorsiflexion. b. McMurray test. c. forefoot adduction. d. knee extension. e. elbow flexion. ANS: D Along with elbows and hips, newborns tend to resist extension of the knee; however, movements should be symmetrical. REF: p. 529 • What technique is performed at every infant examination during the first year of life to detect hip dislocation? a. Ballottement maneuvers b. Barlow-Ortolani maneuvers c. Range of motion d. Thomas McMurray assessment e. Trendelenburg test ANS: B At every examination during an infant’s first year of life, the Barlow-Ortolani maneuver is performed. This test involves stabilizing the pelvis and flexing one hip and knee to 90 degrees. It detects hip dislocation and is signified by a clicking noise with the maneuver. REF: p. 530 • You note that a child has a positive Gower sign. You know that this indicates generalized a. arthropathy. b. muscle weakness. c. bursitis. d. muscle hypertrophy. e. scoliosis. ANS: B Gower sign is generalized muscle weakness and is characterized by a child trying to stand up by flexing at the knee, pushing down on the thighs while trying to pull up the trunk. It is often associated with muscular dystrophy. REF: p. 532 • A 3-year-old boy is brought to the clinic complaining of a painful right elbow. He is holding the right arm slightly flexed and pronated and refuses to move it. The mother states that symptoms started right after his older brother had been swinging him around by his arms. This presentation supports a diagnosis of a. radial head subluxation. b. femoral anteversion. c. carpal tunnel syndrome. d. Osgood-Schlatter disease. e. osteomyelitis. ANS: A The symptoms this child is experiencing are indicative of a radial head subluxation, or nursemaid’s elbow. The symptoms are not consistent with femoral anteversion, carpal tunnel syndrome, Osgood-Schlatter disease, or osteomyelitis. REF: p. 542 • What temporary disorder may be experienced by pregnant women during the third trimester because of fluid retention? a. Carpal tunnel syndrome b. Osteitis deformans c. Radial head subluxation d. Talipes equinovarus e. Legg-Calvé-Perthes disease ANS: A Carpal tunnel syndrome may be experienced by pregnant women during their last trimester because of fluid retention. Fluid retention at the tunnel causes pressure and inflammation at the medial nerve. This results in the symptoms of the syndrome. REF: p. 533 • A red, hot swollen joint in a 40-year-old man should lead you to suspect a. trauma. b. bursitis. c. gout. d. cellulitis. e. tenosynovitis. ANS: C Gout is characterized as red, hot swollen joints, especially the great toe. Gout is commonly linked to men older than 40 years. REF: p. 536 • An adult with bowed tibias and a shortened thorax may have a. ankylosing spondylitis. b. Paget disease. c. rheumatoid arthritis. d. Dupuytren contracture. e. Sprengel deformity. ANS: B Paget disease is characterized by bowed tibias, asymmetric skull, shortened chest, and susceptibility to fractures. REF: p. 537 • In differentiating osteoarthritis from rheumatoid arthritis (RA), the patient with osteoarthritis typically exhibits a. metatarsus adductus. b. depression. c. sudden onset. d. less weakness and fatigue. e. pain most pronounced after periods of rest. ANS: D One of the key differences between the symptoms of osteoarthritis and those of RA is that fatigue is uncommon in osteoarthritis patients. The joints of patients with RA are stiff after rest. REF: p. 538 • A 45-year-old laborer presents with low back pain, stating that the pain comes from the right buttock and shoots down and across the right anterior thigh, down the shin to the ankle. Which examination finding is considered more indicative of nerve root compression? a. Positive straight leg raise result b. Positive Trendelenburg sign c. Negative Romberg test result d. Contralateral straight leg raise result e. Positive drawer test result ANS: D This patient, according to the pattern of radiculopathy, has an L3–L4 injury to the right side. The most alarming finding would be crossover pain to the affected leg while raising the unaffected leg because this finding is more suggestive of herniation. REF: p. 526 • Your examination of an infant reveals a positive Allis sign. To confirm this finding, you would perform a a. startle reflex. b. Barlow-Ortolani maneuver. c. Trendelenburg test. d. tibial torsion test. e. Lachman test. ANS: B The Allis sign will show unequal upper leg lengths, suggestive of a hip dislocation. The Barlow-Ortolani maneuver can confirm results for hip dislocation. REF: p. 530 • A 7-year-old child who begins to limp and complains of persistent hip pain may have a. myelomeningocele. b. Dupuytren contracture. c. Legg-Calvé-Perthes disease. d. osteoarthritis. e. congenital hip dislocation. ANS: C Constant hip pain with a limp in a young child is indicative of Legg-Calvé-Perthes disease. This condition results in avascular necrosis of the femoral head caused by inadequate blood supply. Myelomeningocele, Dupuytren contracture, osteoarthritis, and congenital hip dislocation are not characterized by age group and these symptoms. REF: p. 541 • Dupuytren contracture affects the a. hip flexor muscle. b. plantar fascia. c. carpal tunnel. d. palmar fascia. e. rotator cuff. ANS: D A contracture of the palmar fascia of one or multiple fingers is called a Dupuytren contracture. REF: p. 543 • A dowager hump is a. the hallmark of osteoporosis. b. pathognomic of scoliosis. c. indicative of tendonitis. d. characteristic of rickets. e. indicative of muscular dystrophy. ANS: A Osteoporosis leads to vertebral compression and kyphotic bowing of the spine known as dowager’s hump. REF: p. 543 • Kernig nucal rigidity-meningeal irritation (raise head-involuntary flexion of hips and knees • Thomas test test for flexion contractures of the hips • Lachman tests ACL Anterior cruciate ligament • Romberg used to screen for equilibrium • Cullen sign ecchymosis around the umbilicus • renal calculi signs Abdominal pain on palpation , CVA tenderness, Fever, Hematuria, Nausea • Straight Leg Raising (Bragard's) Raise leg up passively + Pain shooting down leg at 45 degrees - lumbar radiculopathy • Contralateral straight leg raise nerve root compression test and presence of sciatica • Lumbar nerve root irritation L4,L5,S1 + straight leg raise test • Psoas sign Appendicitis - RLQ pain when R thigh is extended (or flexed against resistance) • objective findings of abdominal pain dullness on percussion rebound tenderness • Tingling sensation radiating from the wrist to the hand on striking the median nerve is a positive_______ sign Tinel • Thrombosis of the leg vein Homans- on dorsiflexion of the foot • Murphy sign assess for cholecystitis • Suspect acute appendicitis most unlikely sign consistent RLQ pain • Classic carpal tunnel syndrome reduced abduction of the thumb • Gower's sign Muscle weakness - Duchenne muscular dystrophy - child uses arms to stand up from a squat • Phalen's Test -test for carpal tunnel syndrome -position is held for approximately one minute -if test is positive, pain will be produced in region of carpal tunnel • immune system attacks the synaptic junction between the nerve and muscle fibers blocking acetylcholine receptor sites in Myasthenia gravis • Diabetic neuropathy diminishes pain sensation • Parkinson's disease short shuffling steps • clinical syndrome of intracranial HTN that mimics brain tumors is Pseudotumor Cerebri • A positive Babinski sign is normal until what age? 16 to 24 months • Which of the following is a concern rather than an expected finding in older adults Bilateral pillrolling of the fingers • Bilateral pillrolling is indicative of Parkinson's dx • Ipsilateral Horner syndrome indicates a cerebrovascular accident- CVA occuring in the posterior inferior cerebellar artery • nonspecific infection occurring 10-14 days early primarily affects the motor and autonomic peripheral nerves guillain-Barre • Risk of ovarian cancer is increased by a history of nulliparity • bi-manual examination notes the cervix is positioned posteriorly what would you expect? anteverted • cervical motion tenderness may indicate PID- pelvic inflammatory disease • cervix projecting longer than 5 cm would cause deviated to the left or right • breasts symmetrical with bilateral, freely movable multiple tender masses well defined boarders are consistent with fibrocystic changes • 50 yr old lump firm,fixed,doey-like sign of cancer • found on sides of vestibule in the grove between the labia minora and the hymen Bartholin glands • factors associated with increased risk of cervical cancer early parity • examining the axillary lymph nodes, the patients arms flexed at the elbow • lymphatic flow of the breast primarily drains radially • greatest concern for breast cancer is when you palpate nodes where? supraclavicular • when checking the breast have patient turn their head to the same side that's being examined • examiner uses what when palpating breast tissue? finger pads • largest amount of glandular breast tissue is located where? upper outer quadrant • tail of Spence extends into the axillae • position for examining the breast sit with arms hanging at his/her sides • inspection of breasts begins in what position? Sitting • breast is divided into 4 quadrants plus a tail • conducting a clinical breast examination inspect both breast simultaneously • most common hernia indirect inguinal hernia • least common hernia Femoral hernia and is found mostly in women • risk factor for testicular cancer Cryptorchidiam • expected genitalia change in adult men occurring with age scrotum becomes more pendulos • amount of blood engorging the two corpora cavernosa of the penis when erect 20-50 ml • movement of testes by muscular action regulates testicular temperature • vas deferens male genitalia travels through inguinal canal and unites with seminal vesicle to form ejaculatory duct • male urethral orifice located 2mm ventricle to the tip of the glans • finding associated with recurrent male genital herpes superficial penile vesicles • urethral meatus opens on ventral surface of penis hypospadias • darkly pigmented testes are normal • testicular temperature must be 37 degrees Celsius for what to occur? Spermatogenesis • cheesy white substance on uncircumcised male A collection of sebaceous material called smegma • normal adult testicular size 4x3x2 • greatest contributor to volume of ejaculant prostate • inspection of scrotum should revel the left scrotal sac lower than the right • inspection of the male urethral orifice requires the examiner to press the glans between the thumb and forefinger • When assessing for borborygmi, which physical examination method does the nurse use? a.Inspection b.Palpation c.Auscultation d.Percussion c.Auscultation • penile structure visible to inspection during the physical examination Dorsal vein • uncircumcised male foreskin tight and cannot be easily retracted inquire about previous penile infections • Phimosis Unable to retract the foreskin • technique appropriate for detecting inguinal hernia move finger upward along Vas Deferens • Hernia that lies within the inguinal canal? indirect inguinal hernia • minor consequence in adult male lumps in the scrotum • thick scrotum with edema and pitting indication of general fluid retention • characteristic related to syphilis or diabetic neuropathy is testicular insensitivity to painful stimuli • on palpation a normal vas deferens should feel smooth • premature infants scrotum will appear smooth • enlarged painless testicle in an adolescent or adult male may indicate a tumor • soft, non-tender fullness in scrotum that transluminates hydrocele • What is the most common cancer in men 15-35? Testicular CA • A 16-year-old boy comes to the ED with severe lefttesticular pain and vomiting. Elevation of his left testicle does not lessenthe pain. What could these symptoms indicate for this patient? a) Epididymitis b) Hydrocele c) Testicular cancer d) Lefttesticular torsion d) Lefttesticular torsion • most common hernia in young males indirect inguinal hernia • Difficulty replacing retracted foreskin of penis to its normal position after being retracted behind the glans Paraphimosis • position to examine testicles into scrotum Tailor • difficulty replacing the retracts foreskin of the penis to its normal position is called paraphimosis • genital virus infection known to have a latent phase followed by the production of viral DNA capsids and particles Condyloma acuminatum • condyloma acumination genital warts HPV cauliflower like genital and anal warts increased risk of cervical cancer • smooth, pearly, dome shaped umbilicated papule molluscum contagiosum • Male genital self-examination -perform exam after warm bath or shower -stand naked in front of a mirror -hold penis in your hand and examin the head (pull back foreskin if uncirumcised) -inspect and palpate head of penis in a clockwise motion looking for bumps, sores, or blisters -look for genital wards -look at urethral meatus for discharge -look along entire shaft of penis for same signs -be sure to separate pubic hair at base of penis to examin skin underneith • scrotal mass transluminates with penlight is a hydrocele • condition that is a complication of mumps in an adolescent or adult Orchitis • scrotal swelling signify s (ask parents of small children about scrotal swelling) hernia- • Male with Peyronie dx usually complain of deviation of the penis during erection • Cremasteric Reflex Retraction of the testicle on the stroked side when the inner thigh is stroked. This reflex is absent in testicular torsion (twisting of the testes and spermatic cord). • sexual differentiation of the fetus occurs by 12 weeks gestation • begins with painless, but highly contagious local lesion called a chancre on genitalia syphilis • Solitary, elevated, soft, painless ulcer on the glans or shaft of the penis. Associated with: Primary syphilis • painless induration lesion on glans of penis consistent with chancre • posteriorly the labia minora meet to form fourchette • Cervical Polyp Bright red , soft growth protruding from the endocervical canal • 46) Which of the following are mucus-producing glands located on each side of the vaginal opening? (A) Adrenal (B) Bartholin's (C) Bulbourethral (D) Corpus luteum (E) Parotid Bartholin's • Vaginal Introitus lubricated -Bartholin's Gland • Most common vaginal infection in women of childbearing age BV bacteria in the vagina is disrupted and replaced by an overgrowth of Gardnerella vaginalis Pregnant women w BV - higher risk of preterm delivery Clue Cell, milky discharge RX: metronidazole or clindamycin • vaginal mucosa of a women with childbearing years appears transversely rugated • adnexa uterine tubes and ovaries • Bluish purple discoloration of the cervix, vagina, and labia during pregnancy as a result of increased vascular congestion? Chadwick's sign • pelvic joints that separates most during late pregnancy symphysis • pregnancy related cervical changes softening and blueish color • conventional defination of menopause no period for 1 year • related effects of menopause increased abdominal fat distribution • menopause increase LDL,Cholesterol, intra-abdominal body fat , and hot flashes • hx of vaginal discharge and itching what would you ask when obtaining an H&P Douching routine • Lifestyle factors associated with increased risk of cervical cancer 1. Early onset of sexual activity 2. Multiple sexual partners 3. Exposure to high risk partners 4. History of STDs 5. Smoking 6. High parity 7. Prolonged use of oral contraception • ovarian cancer risks increase with use of oral contraceptives • obese women have an increased risk for: (4) gallbladder cancer biliary passage cancer breast cancer cervical, endometrial, ovarian cancer • discharge stain on 8 yr old underwear would indicate risk for sexual abuse • pelvic exam position lithotomy • speculum inserted for cytologic studies with lubrication of warm water • possible gonococcal infection discharge fro urethra or Skene gland • change gloves after examining anal area • cervix positioned posteriorly-bimanual exam would expect to palpate an anteverted uterus • Cervical motion tenderness (chandelier sign), purulent cervical discharge PID • proper speculum technique during exam press down on introitus downward and insert closed speculum obliquely • Small, white or yellow, raised round areas on the cervix are known as ____ Nabothian cysts (considered normal) • brush withdrawn from cervical os and sample applied to slide with fixative added cytology smear • when collecting vaginal samples what is collected first pap smear • Dacron swabs for Chlamydia • Clue cells Bacterial vaginosis • Fishy odor Bacterial vaginosis • bimanual exam of uterus includes grasping the cervix between the examining fingers • strength of the trapezius muscle is evaluated by having the patient push her or his head against the examiner's hand • expected normal findings during the inspection of spinal alignment incude the head positioned superiorly to the gluteal cleft • __ is common in patients who are markedly obese or pregnant. Lordosis • a wheelchair- dependent older women would most likely develop skin breakdown at the gibbus • patient flexes forward at the waist , which spinal observation would lead to laternal curvature of the spine • The autonomic nervous system coordinates which of the following? a. High-level cognitive function b. Balance and affect c. Internal organs of the body d. Balance and equilibrium e. Emotions and behavior ANS: C The autonomic nervous system coordinates the internal organs of the body by the sympathetic and parasympathetic nervous systems. The other options are associated with the cerebral cortex, whose function consists of determining intelligence, personality, and motor function. REF: p. 544 • The major function of the sympathetic nervous system is to a. orchestrate the stress response. b. coordinate fine motor movement. c. determine proprioception. d. contribute input from visual, labyrinthine, and proprioceptive sources. e. perceive stereognosis. ANS: A Stimulation of the sympathetic branch of the autonomic nervous system prepares the body for emergencies for fight or flight (stress response). The cerebellum plays a key role in the coordination of fine motor movements. Recognition of body parts and awareness of body position (proprioception) are dependent on the parietal lobe. The basal ganglia contribute input from visual, labyrinthine, and proprioceptive sources. Stereognosis is the ability to perceive weight and form of solid objects by touch and is not under sympathetic control. REF: p. 544 • The parasympathetic nervous system maintains the day-to-day function of a. digestion. b. response to stress. c. lymphatic supply to the brain. d. lymphatic drainage of the brain. e. coordinating fine motor movements. ANS: A The parasympathetic division functions in a complementary and a counterbalancing manner to conserve body resources and maintain day-to-day body functions such as digestion and elimination. REF: p. 544 • Cerebrospinal fluid serves as a a. motor nerve impulse transmitter. b. red blood cell conveyer. c. shock absorber. d. mediator of voluntary skeletal movement. e. sensory nerve impulse transmitter. ANS: C Cerebrospinal fluid circulates between an interconnecting system of ventricles in the brain and around the brain and spinal cord, serving as a shock absorber. Neurotransmitters are chemicals that transmit nerve impulses from one nerve cell to another. The cerebrospinal fluid does not play a role in red blood cells or in voluntary skeletal movement. REF: p. 545 • The motor cortex of the brain is in the a. corpus callosum. b. frontal lobe. c. limbic system. d. occipital lobe. e. parietal lobe. ANS: B The frontal lobe contains the motor cortex associated with voluntary skeletal movement and fine repetitive motor movements, as well as the control of eye movements. The corpus callosum interconnects the counterpart areas in each hemisphere, unifying the cerebrum’s higher sensory and motor functions. The limbic system mediates the sense of smell and certain patterns of behavior that determine survival, such as mating, aggression, fear, and affection. The occipital lobe contains the primary vision center and provides interpretation of visual data. The parietal lobe is primarily responsible for processing sensory data as they are received. REF: p. 546 • The thalamus is the major integration center for perception of a. speech. b. olfaction. c. pain. d. thoughts. e. visceral responses to emotions. ANS: C The thalamus is the major integrating center for perception of various sensations such as pain and temperature, serving as the relay center between the basal ganglia and cerebellum. The reception of speech and interpretation of speech is located in the Wernicke area. The olfactory sense is processed in the parietal lobe. The cerebrum holds memories, allows you to plan, and enables you to imagine and think. The limbic system mediates the sense of smell and certain patterns of behavior (primitive behaviors, visceral response to emotional and biologic rhythms) that determine survival, such as mating, aggression, fear, and affection. REF: p. 546 • The awareness of body position is known as a. extrapyramidal. b. graphesthesia. c. stereognosis. d. two-point discrimination. e. proprioception. ANS: E Recognition of body parts and awareness of body position is known as proprioception. This is dependent on the parietal lobe. REF: p. 546 • Which area of the brain is responsible for perceiving sounds and for determining their source? a. Frontal lobe b. Occipital lobe c. Parietal lobe d. Temporal lobe e. Brainstem ANS: D The temporal lobe is responsible for the perception and interpretation of sounds and determination of their source. The frontal lobe contains the motor cortex associated with voluntary skeletal movement. The occipital lobe contains the primary vision center. The parietal lobe is primarily responsible for processing received sensory data. The brainstem is the pathway between the cerebral cortex and the spinal cord, and it controls many involuntary functions. REF: p. 546 • Nerves that arise from the brain rather than the spinal cord are called a. sympathetic. b. parasympathetic. c. cranial. d. autonomic. e. lower motor neurons. ANS: C Cranial nerves are peripheral nerves that arise from the brain rather than the spinal cord. Sympathetic, parasympathetic, and autonomic refer to the autonomic nervous system. Lower motor neurons arise in the spinal cord. REF: p. 547 • If a patient cannot shrug the shoulders against resistance, which cranial nerve (CN) requires further evaluation? a. CN I, olfactory b. CN V, trigeminal c. CN IX, glossopharyngeal d. CN XI, spinal accessory e. CN XII, hypoglossal ANS: D CN XI is responsible for the motor ability to shrug the shoulders. CN I is associated with smell reception and interpretation. CN V is associated with opening of the jaw; chewing; and sensation of the cornea, iris, conjunctiva, eyelids, forehead, nose, teeth, tongue, ear, and facial skin. CN IX is associated with swallowing function, sensation of the nasopharynx, gag reflex, taste, secretion of salivary glands, carotid reflex, and swallowing. CN XII is associated with movement of the tongue. REF: p. 553 • The major portion of brain growth and myelinization occurs between ____ year(s) of age. a. birth and 1 b. 2 and 3 c. 4 and 7 d. 11 and 14 e. 16 and 21 ANS: A The major portion of brain growth occurs in the first year of life along with myelinization of the brain and nervous system. REF: p. 549 • Motor maturation proceeds in an orderly progression from a. peripheral to central. b. head to toe. c. lateral to medial. d. pedal to cephalic. e. toe to head. ANS: B Motor maturation proceeds in a cephalocaudal direction. Motor control of the head and neck develops first followed by the trunk and extremities. The other choices are incorrect because they relate maturation sequence inappropriately. REF: p. 549 • Normal changes of the aging brain include a. increased velocity of nerve conduction. b. diminished perception of touch. c. increased total number of neurons. d. decreased dermatomes. e. diminished intelligence quotient. ANS: B Sensory perceptions of touch and pain are diminished by aging. The velocity of nerve impulse conduction declines, so response to stimuli takes longer. The number of cerebral neurons is thought to decrease by 1% a year beginning at 50 years of age; however, the vast number of reserve cells inhibits the appearance of clinical signs. Dermatomal patterns do not change. Acquired knowledge is maintained throughout life. REF: p. 549 • The area of body surface innervated by a particular spinal nerve is called a a. dermatome. b. nerve pathway. c. spinal accessory area. d. cutaneous zone. e. spinal tract. ANS: A The sensory and motor fibers of each spinal nerve supply and receive information to a segment of skin known as a dermatome. Nerve pathway and spinal accessory area refer to nerve routes; cutaneous zone refers to a skin area that transmits fine mechanical information and normal exogenous thermal information at the same time. Spinal tracts are located in the spinal cord. REF: p. 547 • Environmental hazards and cognitive function are data needed for the personal and social history section of a neurologic assessment for a. adolescents. b. every patient. c. persons with seizures. d. pregnant women. e. infants. ANS: B Exposure to lead, arsenic, insecticides, organic solvents, dangerous equipment, and work at heights or in water are important factors to consider in the personal and social history of all patients. REF: p. 551 • A neurologic past medical history should include data about a. family patterns of dexterity and dominance. b. circulatory problems. c. educational level. d. immunizations. e. allergies. ANS: B The neurologic past medical history should include data concerning neurovascular problems such as stroke, aneurysm, and brain surgery. The other answers are not pertinent medical information for the neurologic past medical history. REF: p. 551 • When assessing superficial pain, touch, vibration, and position perceptions, you are testing a. motor function. b. cerebellar function. c. sensory function. d. tendon reflexes. e. emotional status. ANS: C Superficial pain, touch, vibration, and position perceptions are sensory functions. Cerebellar function and tendon reflexes are neuromuscular functions, and emotional status is regulated in the amygdala within the temporal lobe. REF: p. 561 • You are examining a patient in the emergency department who has recently sustained head trauma. To initially assess this patient’s neurologic status, you would a. ask him to discriminate between the smell of orange and peppermint. b. test the six cardinal points of gaze. c. palpate the jaw muscles as the patient clenches teeth. d. observe for swallowing and test the gag reflex. e. test the patient’s tongue movements. ANS: B The sixth cranial nerve is commonly one of the first to lose function in the presence of increased intracranial pressure. Testing of the six cardinal points of gaze involves CN VI, which would be a priority. REF: p. 554 • You are initially evaluating the equilibrium of Ms. Q You ask her to stand with her feet together and arms at her sides. She loses her balance. Ms. Q has a positive a. Kernig sign. b. Homan sign. c. McMurray test. d. Romberg sign. e. Murphy sign. ANS: D The Romberg test has the patient stand with his or her eyes closed, feet together, and arms at the sides. Slight swaying movement of the body is expected but not to the extent of falling. Loss of balance results in a positive Romberg test. Kernig sign tests for meningeal irritation, Homan sign tests for venous thrombosis, and McMurray test is a rotation test for demonstrating a torn meniscus. A positive Murphy sign is usually a sign of gallbladder disease. REF: p. 559 • The finger-to-nose test allows assessment of a. coordination and fine motor function. b. point location. c. sensory function. d. two-point discrimination. e. stereognosis. ANS: A To perform the finger-to-nose test, the patient closes both eyes, and touches his or her nose with the index finger, alternating hands while gradually increasing the speed. This tests coordination and fine motor skills. All of the other choices test sensory function without motor function. REF: p. 557 • You are performing a two-point discrimination test as part of a well physical examination. The area with the ability to discern two points in the shortest distance is the a. back. b. palms. c. fingertips. d. upper arms. e. chest. ANS: C On the fingertips and toes, two points are commonly felt when 2 to 8 mm apart. A greater distance is expected for discrimination of two points on other body parts, such as the back (40 to 70 mm) or chest and forearms (40 mm). REF: p. 562 • As Mr. B enters the room, you observe that his gait is wide based and he staggers from side to side while swaying his trunk. You would document Mr. B’s pattern as a. dystonic ataxia. b. cerebellar ataxia. c. steppage gait. d. tabetic stamping. e. Parkinsonian gait. ANS: B A cerebellar gait (cerebellar ataxia) occurs when the patient’s feet are wide based with a staggering gait, lurching from side to side, often accompanied by swaying of the trunk. Dystonic ataxia is jerky dancing movements that appear nondirectional. Steppage gait is noted when the hip and knee are elevated excessively high to lift the plantar flexed foot off the ground. The foot is brought down with a slap, and the patient is unable to walk on the heels. Tabetic stamping occurs when the legs are positioned far apart, lifted high, and forcibly brought down with each step; in this case, the heel stamps on the ground. In Parkinsonian gait, the patient’s posture is stooped, and the body is held rigid; steps are short and shuffling, with hesitation on starting and difficulty stopping. REF: p. 559 • Deep pressure tests are used mostly for patients who are experiencing a. absent superficial pain sensation. b. gait and stepping disturbances. c. lordosis, osteoporosis, or arthritis. d. brisk reflexes. e. tonic neck or torso spasms. ANS: A Deep pressure sensation is tested by squeezing the trapezius, calf, or biceps muscle, thus causing discomfort. When superficial pain sensation is not intact, then further assessments of temperature and deep pressure sensation are performed. REF: p. 561 • To assess a cremasteric reflex, the examiner strokes the a. skin around the anus and observes for the anal wink. b. abdomen and observes whether the umbilicus moves away from the stimulus. c. inner thigh and observes whether the testicle and scrotum rise on the stroked side. d. palm and observes whether the fingers attempt to grasp. e. sole of the foot and observes whether the toes fan down and out. ANS: C Stroking the inner thigh of a male patient (proximal to distal) will elicit the cremasteric reflex. The testicle and scrotum rise on the stroked side. Stoking the skin around the anus produces reflexive contracture of the external anal sphincter referred to as the anal wink. Stroking the sole of the foot elicits a Babinski sign, stroking the abdomen elicits an abdominal reflex, and stroking the palm elicits a palmar grasp. REF: p. 562 • You have asked a patient to close his eyes and identify an object placed in his hand. You are evaluating a. stereognosis. b. graphesthesia. c. vibratory sense. d. two-point discrimination. e. extinction phenomenon. ANS: A Stereognosis is the ability to recognize an object through touch and manipulation. Tactile agnosia, an inability to recognize objects by touch, suggests a parietal lobe lesion. Graphesthesia tests the patient’s ability to identify the figure being drawn on his or her palm. The vibratory sense uses a tuning fork placed on a bony prominence. Two-point discrimination uses two sharp objects to determine the distance at which the patient can no longer distinguish the two points. The extinction phenomenon tests sensation by simultaneously touching bilateral sides of the body with a sterile needle. REF: p. 562 • The ability to recognize a number traced on the skin is called a. stereognosis. b. graphesthesia. c. extinction phenomenon. d. two-point discrimination. e. proprioception. ANS: B The ability to recognize a number traced on the skin is called graphesthesia. Stereognosis is the ability to recognize an object through touch and manipulation. The extinction phenomenon test and two-point discrimination assess the person’s ability to discern the number of pinpoints and their location. Proprioception is the sensation of position and muscular activity originating from within the body. REF: p. 562 • Which one of the following conditions is consistent with Brown-Séquard syndrome? a. Central sensory loss that is generalized b. Motor paralysis on lesion side of the body c. Multiple peripheral neuropathy of the joints d. Spinal root paralysis below the umbilicus e. Pain and temperature loss on lesion side of body ANS: B Partial spinal sensory syndrome (Brown-Séquard syndrome) is noted when pain and temperature sensation loss occur one to two dermatomes below the lesion on the opposite side of the body from the lesion. Proprioceptive loss and motor paralysis occur on the lesion side of the body. REF: p. 562 • To assess spinal levels L2, L3, and L4, which deep tendon reflex should be tested? a. Triceps b. Patellar c. Biceps d. Achilles e. Brachioradial ANS: B To assess spinal levels L2 to L4, the patellar reflex should be tested. The patellar tendon is the only deep tendon that assesses the lumbar spinal level. The triceps, biceps, and brachioradial deep tendon reflexes are tested to assess the cervical spine, and the Achilles tendon is tested to assess the sacral spine. REF: p. 563 • When using a monofilament to assess sensory function, the examiner a. uses two simultaneous monofilaments on similar bilateral points and then compares results. b. applies both a monofilament and a pin on similar bilateral points and then compares results. c. applies pressure to the monofilament until the filament bends. d. strokes the monofilament along the skin from proximal to distal areas. e. assesses only the dorsal surface of the foot with the patient’s eyes open. ANS: C The monofilament is placed on several smooth spots of the patient’s plantar foot for 1 seconds. Adequate pressure applied by the monofilament is measured by the bend of the monofilament. REF: p. 565 • Visible or palpable extension of the elbow is caused by reflex contraction of which muscle? a. Serratus anterior b. Biceps c. Pectoralis major d. Triceps e. Deltoid ANS: D The triceps tendon, when directly hit with the reflex hammer just above the elbow, will cause contraction of the triceps muscle and extension of the elbow. REF: p. 564 • It is especially important to test for ankle clonus if a. deep tendon reflexes are hyperactive. b. the patient has a positive Kernig sign. c. the Romberg sign is positive. d. the patient has peripheral neuropathy. e. deep tendon reflexes are hypoactive. ANS: A Test the ankle clonus when reflexes are hyperactive. Support the patient’s knee in a flexed position and briskly dorsiflex the foot with your other hand. If clonus is present, there is recurrent ankle plantar flexion movement as long as the examiner retains the foot in dorsiflexion. Sustained clonus signifies the hypertonia of an upper motor neuron lesion. REF: p. 565 • Which sign is associated with meningitis and intracranial hemorrhage? a. Babinski sign b. Asymmetric tonic neck reflex c. Doll’s eye movement d. Nuchal rigidity e. Moro reflex ANS: D A stiff neck or nuchal rigidity is a sign associated with meningitis and intracranial hemorrhage. Test this by lifting the head of the patient to touch the chin while the patient lies in a supine position. Pain and resistance to neck motion are associated with nuchal rigidity. All of the other options are expected findings in infants and are not related to meningitis in adults. REF: p. 565 • When assessing a 17-year-old patient for nuchal rigidity, you gently raise his head off the examination table. He involuntarily flexes his hips and knees. To confirm your suspicions associated with this positive test result, you would also perform a test for the _____ sign. a. Kernig b. Babinski c. obturator d. Brudzinski e. Murphy ANS: A The first action elicited the Brudzinski sign. This sign is an indicator of meningeal irritation. To confirm meningeal irritation, you would test for the Kerning sign, also a meningeal sign. REF: p. 566 • On a scale of 0 to 4+, which deep tendon reflex score is appropriate for a finding of clonus in a patient? a. 0 b. 1+ c. 2+ d. 3+ e. 4+ ANS: E 0 indicates absent reflexes; 1+ indicates sluggish or diminished reflex; 2+ indicates active or expected response; 3+ indicates more brisk than expected, slightly hyperactive; and 4+ indicates brisk, hyperactive, with intermittent or transient clonus. REF: p. 564 • Cranial nerve XII may be assessed in an infant by a. watching the infant’s facial expressions when crying. b. observing the infant suck and swallow. c. clapping hands and watching the infant blink. d. observing the infant’s rooting reflex. e. checking the infant’s gag reflex. ANS: B Cranial nerve (CN) XII may be assessed in an infant by observing the infant suck and swallow and by pinching the nose and then observing for the mouth to open and the tip of the tongue to rise in a midline position. Watching the infant’s facial expressions when crying assesses CN VII, clapping hands and watching the infant blink tests CN VIII, and observing the rooting reflex assesses CN V. A gag reflex assesses CN IX and X. REF: p. 567 • At what age should an infant begin to transfer objects from hand to hand? a. 2 months b. 4 months c. 7 months d. 10 months e. 12 months ANS: C Transferring objects hand to hand begins at 7 months. Purposeful release of objects is noted as a normal finding by 10 months. Purposeful movements, such as reaching and grasping for objects, begin at about 2 months of age. The progress of taking objects with one hand begins at 6 months. There should be no tremors or constant overshooting of movements. REF: p. 566 • A positive Babinski sign is normal until what age? a. 3 to 6 months b. 9 to 15 months c. 16 to 24 months d. 3 years e. 5 years ANS: C A positive Babinski sign, fanning of the toes and dorsiflexion of the great toe, is a normal finding until the infant is 16 to 24 months old. REF: p. 568 • Which of the following is a concern, rather than an expected finding, in older adults? a. Reduced ability to differentiate colors b. Bilateral pillrolling of the fingers c. Absent plantar reflex d. Diminished senses of smell and taste e. Reduced gag reflex ANS: B Bilateral pillrolling is indicative of Parkinson disease; the other choices are expected findings with aging. REF: p. 579 • Ipsilateral Horner syndrome indicates a cerebrovascular accident (CVA) occurring in the a. anterior spinal artery. b. internal or middle cerebral artery. c. posterior inferior cerebellar artery. d. vertebral or basilar arteries. e. anterior portion of the pons. ANS: C The posterior inferior cerebellar artery supplies the lateral and posterior portion of the medulla. A CVA involving this artery can produce a neurologic sign of ipsilateral Horner syndrome in the eye. REF: p. 576 • An acute polyneuropathy that commonly follows a nonspecific infection occurring 10 to 14 days earlier and that primarily affects the motor and autonomic peripheral nerves in an ascending pattern is a. cerebral palsy. b. HIV encephalopathy. c. Guillain-Barré syndrome. d. Rett syndrome. e. myasthenia gravis. ANS: C Guillain-Barré syndrome (acute idiopathic polyneuritis) is an acute polyradiculoneuropathy that commonly follows a nonspecific infection that occurred 10 to 14 days earlier. It is characterized by ascending symmetrical weakness with sensation preserved. An increase in the severity occurs over days or weeks. A decrease or absent strength and sensory loss may result along with motor paralysis and respiratory muscle failure. REF: p. 577 • The immune system attacks the synaptic junction between the nerve and muscle fibers blocking acetylcholine receptor sites in a. myasthenia gravis. b. encephalitis. c. multiple sclerosis. d. cerebral palsy. e. trigeminal neuralgia. ANS: A Myasthenia gravis is a chronic autoimmune neuromuscular disease involving the lower motor neurons and muscle fibers. The immune system of infected individuals produces antibodies that destroy acetylcholine receptor sites at the neuromuscular junction. This blocks the nerve impulse from reaching the muscle and produces muscle fatigue. REF: p. 576 • Diabetic peripheral neuropathy will likely produce a. hyperactive ankle reflexes. b. diminished pain sensation. c. exaggerated vibratory sense. d. hypersensitive temperature perception. e. exaggerated sharp touch sensation. ANS: B Peripheral neuropathy is a disorder of the peripheral nervous system that results in motor and sensory loss in the distribution of one or more nerves, more commonly in the hands and feet. Patients may have sensation of numbness, tingling, burning, and cramping. In moderate to severe diabetic neuropathy, the patient has wasting of the foot muscles, absent ankle and knee reflexes, decreased or no vibratory sensation below the knees, or loss of pain or sharp touch sensation to the mid-calf level. REF: p. 578 • Persons with Parkinson disease have an altered gait that is characterized by a. short shuffling steps. b. the trunk in a backward position. c. exaggerated swinging of the arms. d. lifting the legs in a high-step fashion. e. wide-based, staggering, and lurching steps. ANS: A The altered gait of Parkinson disease has short shuffling steps, the posture is stooped forward, and the arms have limited swing. REF: p. 579 • A clinical syndrome of intracranial hypertension that mimics brain tumors is a. meningitis. b. myasthenia gravis. c. Guillain-Barré syndrome. d. pseudotumor cerebri. e. Bell palsy. ANS: D Pseudotumor cerebri is a clinical syndrome of intracranial hypertension that mimics brain tumors. Its cause is unknown, but one theory is that an impaired venous outflow leads to increased cerebral blood volume; it may also be idiopathic. REF: p. 574 • When auscultating the apex of the lung, you should listen a. even with the second rib. b. 4 cm above the first rib. c. higher on the right side. d. on the convex diaphragm surface. e. directly over the clavicles. ANS: B The apices of the lungs are 4 cm above the first rib. REF: p. 262 • You are documenting a rash between the eighth and ninth ribs on the lateral border. This intercostal space will be documented in terms of the a. rib immediately above it. b. rib immediately below it. c. number of centimeters it is positioned below the clavicle. d. number of inches it is positioned below the clavicle. e. relationship to the sternum. ANS: A The number of each intercostal space corresponds to that of the rib immediately above it. REF: p. 263 • To begin counting the ribs and the intercostal spaces, you begin by palpating the reference point of the a. distal point of the xiphoid. b. manubriosternal junction. c. suprasternal notch. d. acromion process. e. clavicle. ANS: B The angle of Louis, the junction of the manubrium and the sternum, corresponds to the second rib, the reference point for counting ribs and intercostal spaces. REF: p. 263 • Fetal gas exchange is mediated by the a. pleura. b. heart. c. amniotic fluid. d. placenta. e. lungs. ANS: D The placenta is the source for fetal gas exchange; the lungs contain no air, and the alveoli are collapsed. REF: p. 264 • The foramen ovale should close by a. 24 weeks of gestation. b. the initiation of labor. c. within minutes of birth. d. 4 weeks of age. e. 12 months of age. ANS: C The decrease in pulmonary pressures within the first minutes of life leads to closure of the foramen ovale. REF: p. 264 • Increased oxygen tension in the arterial blood of a newborn infant causes a. closure of the ductus arteriosus. b. hyperinflation of the lungs. c. passive respiratory movements. d. reopening of the foramen ovale. e. the pulmonary arteries to contract. ANS: A Increased oxygen tension in the arterial blood usually stimulates contraction and closure of the ductus arteriosus. REF: p. 264 • The anteroposterior diameter of the chest is normally approximately the same as the transverse diameter in which age group? a. Infants b. School-age children c. Adolescents d. Young adults e. Older adults ANS: A The chests of infants are generally round, with equal dimensions of anteroposterior and transverse diameters. REF: p. 264 • To accommodate the enlarging uterus of pregnancy, the chest changes result in a. intercostal muscle atrophy. b. lowering of the resting diaphragm. c. decreased alveoli expansion. d. decreased diaphragmatic movement. e. increased costal angle. ANS: E The costal angle progressively increases from approximately 68.5 degrees to 103.5 degrees in later pregnancy. The resting diaphragm rises, yet diaphragmatic movement increases, the alveolar ventilation and tidal volume increase, and the muscles do not atrophy. REF: p. 265 • The characteristic barrel chest of an older adult is caused by a combination of factors, including a. skeletal changes of aging. b. increased muscular expansion of the chest wall. c. less fibrous alveoli. d. increased vital capacity. e. increased lung resiliency. ANS: A Skeletal changes associated with aging include an emphasis of the dorsal curve of the thoracic spine that contributes to a barrel chest. REF: p. 265 • Nancy is a 16-year-old young woman who presents to the clinic with complaints of severe, acute chest pain. Her mother reports that Nancy, apart from occasional colds, is not prone to respiratory problems. What potential risk factor is most important to assess concerning Nancy’s present problem? a. Anorexia symptoms b. Illegal drug use c. Last menses d. Signs of rheumatic fever e. Sexual activity ANS: B Illegal drug use, particularly of cocaine, is especially important to prioritize as a social history question for all adolescents and adults who complain of severe chest pain. Cocaine use can lead to tachycardia, hypertension, coronary arterial spasm with infarction, and pneumothorax. REF: p. 267 • A patient describes shortness of breath that gets worse when he sits up. Which term documents this? a. Platypnea b. Orthopnea c. Tachypnea d. Bradypnea e. Hypopnea ANS: A Dyspnea that increases in the upright posture is called platypnea. Orthopnea is dyspnea that worsens with lying down, tachypnea is increased respiratory rate, and bradypnea is decreased respiratory rate. Hypopnea refers to abnormally shallow respirations. REF: p. 266 • Bradypnea may accompany a. pneumothorax. b. an excellent level of cardiovascular fitness. c. ascites. d. a pulmonary embolus. e. anxiety. ANS: B Bradypnea, a rate slower than 12 breaths/min, may result from cardiorespiratory fitness. The other choices accompany tachypnea. REF: p. 270 • A 34-year-old man is being seen for complaints of dull pain between the shoulder blades that is more intense with deep breathing and coughing. Upon auscultation of the chest, you suspect that you will hear a. rhonchi. b. expiratory wheeze. c. crackles. d. pleural friction rub. e. crepitus. ANS: A This patient is describing the bronchi as the source of the pain; the trachea divides at T4–5, between the shoulder blades. The adventitious bronchial sound expected is rhonchi. Wheezing might be expected if the patient had productive coughing or dyspnea; a pleural friction rub usually causes sudden stabbing pain over the pleuritic site. Crepitus can be both palpated and heard; it indicates air in the subcutaneous tissue and is usually found anteriorly and toward the axilla. REF: p. 279 • The most appropriate lighting source to highlight chest movement is (are) a. bright tangential lighting. b. daylight from a window. c. flashlight in a dark room. d. fluorescent ceiling lights. e. a Wood’s lamp. ANS: A Bright tangential light is best to visualize chest movements. REF: p. 268 • Both pleural effusion and lobar pneumonia are characterized by _____ percussion. a. tympany heard with b. dullness heard on c. resonance heard on d. hyperresonance heard on e. occasional hyperresonance heard on ANS: B Pleural effusion and lobar pneumonia are more dense than air, with an expected finding of dullness to percussion. Tympany is expected over hollow organs such as the stomach; resonance and hyperresonance are heard over air-filled areas. REF: p. 274 • Which finding suggests a minor structural variation? a. Barrel chest b. Clubbed fingers c. Pectus carinatum d. Retractions e. Tachypnea ANS: C Barrel chest, clubbed fingers, chest wall retractions, and tachypnea result from compromised respirations; pectus carinatum (pigeon chest) is a minor structural variation. REF: p. 268 • Ms. R, age 74 years, has no known health problems or diseases. You are doing a preventive health care history and examination. Which symptom is associated with an intrathoracic infection? a. Barrel chest b. Cor pulmonale c. Pectus excavatum d. Pectus carinatum e. Malodorous breath ANS: E Intrathoracic infections may make the breath malodorous; the other conditions will not. REF: p. 273 • In barrel chest, the ratio of the anteroposterior diameter to the transverse (lateral) diameter is a. 0.7 to 0.75. b. 1.0. c. 1.3 to 1.5. d. 1.5 to 2. e. greater than 2. ANS: B In a barrel chest, an increase in the chest anteroposterior diameter leads to an increase in the thoracic ratio (anteroposterior to transverse diameters) of 1.0, in which the chest is equally wide as it is thick. REF: p. 265 • The patient that you are examining is complaining of pain near the spine. While palpating the spinous process at T7 and medially to the inferior border of the right scapula, the patient feels more intense pain. When viewing the chest radiograph, you will carefully look at which rib? a. Right sixth rib b. Right seventh rib c. Right eighth rib d. Left seventh rib e. Left eighth rib ANS: C Although each rib articulates with the corresponding vertebra, the palpated spinous process dips down so that the rib you feel in apparent association with the spinous process is actually the number of that process plus 1. REF: p. 263 • The best time to observe and count respirations is a. while the patient is answering questions. b. while weighing the patient. c. after palpating the pulse. d. when the patient is sleeping. e. after a short walk. ANS: C Respiratory patterns change as the patient speaks and sleeps. Attempting to count during weighing would make the patient self-conscious and affect the respiratory rate. Counting respirations after you palpate the pulse does not make the patient self-conscious because the patient expects you to be counting the pulse. REF: p. 270 • As you take vital signs on Mr. B, age 78 years, you note that his respirations are 40 breaths/min. He has been resting, and his mucosa is pink. Concerning Mr. B’s respirations, you would a. document his rate as normal. b. do nothing because his color is pink. c. note that his rate is below normal. d. report that he has an above-average rate. e. ignore one abnormal result. ANS: D The normal adult respiratory rate is 12 to 20 breaths/min, with a ratio of respirations to heartbeats of 1:4. Always note any variations in respiratory rate. REF: p. 270 • In which patient situation would you expect to assess tachypnea? a. Patient with depression b. Patient who abuses narcotics c. Patient with metabolic acidosis d. Patient with myasthenia gravis e. Patient with metabolic alkalosis ANS: C In metabolic acidosis, the body compensates by increasing the respiratory rate to blow off the excess carbon dioxide. The other choices cause respiratory depression. REF: p. 270 • What term would you use to document a respiratory rate greater than 20 breaths/min in an adult? a. Dyspnea b. Orthopnea c. Platypnea d. Tachypnea e. Cheyne-Stokes ANS: D Tachypnea is the correct term for respirations greater than 20 breaths/min. Dyspnea, orthopnea, and platypnea are terms that describe respiratory effort, not rate. Cheyne-Stokes refers to a particular abnormal pattern of respiration. REF: p. 270 • Respiratory effort usually exhibited by the patient with cerebral brain damage is called a. Cheyne-Stokes respiration. b. paroxysmal nocturnal dyspnea. c. Kussmaul breathing. d. Biot respiration. e. ataxic respiration. ANS: A Cheyne-Stokes respirations occur in children and older adults during sleep but otherwise occur in seriously ill patients, particularly those with brain damage at the cerebral level. The other choices are not apnea associated with cerebral damage. REF: p. 271 • Which site of chest wall retractions indicates a more severe obstruction in a patient with asthma? a. Lower chest b. Along the anterior axillary line c. Above the clavicles d. At the nipple line e. Along the posterior axillary line ANS: C Asthma more commonly produces retractions of the lower chest. The more severe the obstruction, the greater is the negative pressure produced in the chest during inspiration and retractions are seen in the upper thorax. REF: p. 282 • Which type of apnea requires immediate action? a. Primary apnea b. Secondary apnea c. Sleep apnea d. Periodic apnea of the newborn e. Apnea of prematurity ANS: B Primary apnea is self-limiting, sleep apnea should be evaluated but does not require immediate action, and periodic apnea of the newborn is a normal condition. Apnea of prematurity is a more intense version of periodic apnea of the newborn. Secondary apnea is grave, and unless resuscitative measures are immediately instituted, breathing will not resume spontaneously. REF: p. 271 • Laryngeal obstructions would elicit which breath sound? a. Fremitus b. Stridor c. Rhonchi d. Crepitus e. Wheezing ANS: B Obstructions high in the respiratory tree are characterized by stridor. REF: p. 272 • Mr. L has cyanotic lips and nail beds. His lips are pursed, and he has nasal flaring. You suspect that he has cardiac or pulmonary difficulty. What additional sign would correspond with your impression? a. Callus formation on the heels b. Clubbing of the fingers c. Graying of the hair d. Swollen toes and ankles e. Positioning of the head ANS: B Clubbing of the fingers suggests chronic pulmonary or cardiac difficulty. The other choices do not. REF: p. 273 • Breath odors may alert the examiner to certain underlying metabolic conditions. The odor of ammonia on the breath may signify a. uremia. b. tuberculosis. c. hepatic dysfunction. d. diabetic ketoacidosis. e. intestinal obstruction. ANS: A The breath smell described as ammonia-like suggests uremia, a renal condition; cinnamon suggests tuberculosis, a musty fish or clover odor suggests hepatic failure, a sweet and fruity odor suggests diabetic ketoacidosis; and a foul or feculent odor suggests intestinal obstruction. REF: p. 277 • An expected finding from chest palpation in the adult would be a. costal angle of 120 degrees. b. cracking over the sternal notch. c. greater right chest expansion. d. crepitus. e. inflexibility of the xiphoid. ANS: E The sternum and xiphoid in adults are relatively inflexible, without cracking; the expected normal costal angle is 90 degrees, and the chest moves symmetrically. Crepitus is always an abnormal finding. REF: p. 273 • You would expect to document the presence of a pleural friction rub for a patient being treated for a. bronchitis. b. atelectasis. c. pleurisy. d. emphysema. e. pneumonia. ANS: C A pleural friction rub is caused by inflammation of the pleural surfaces and is expected to be auscultated with pleurisy. REF: p. 280 • Tactile fremitus is best felt a. along the costal margin and xiphoid process. b. in the suprasternal notch along the clavicle. c. at the level of bifurcation of the bronchi. d. posterolaterally over the scapulas. e. in the midaxillary lines. ANS: C Fremitus is best felt posteriorly and laterally at the level of the bifurcation of the bronchi. There is great variability depending on the intensity and pitch of the voice and the structure and thickness of the chest wall. In addition, the scapulae obscure fremitus. REF: p. 273 • In the most effective percussion technique of the posterior lung fields, the patient cooperates by a. folding the arms in front. b. bending the head back. c. standing and bending forward. d. lying on the side and extending the top arm. e. lying prone. ANS: A Asking the patient to sit with the head forward and arms folded in front moves the scapula laterally, exposing more lung to percussion. REF: p. 274 • The examiner percusses for diaphragmatic excursion along the a. vertebral column. b. midvertebral line. c. midaxillary line. d. scapular line. e. sternum. ANS: D The technique for diaphragmatic excursion is to percuss along the scapular line, after the patient inhales deeply, and to mark the site when resonance changes to dullness, representing the diaphragm. The sequence is repeated with exhalation. REF: p. 276 • The diaphragm of the stethoscope is better than the bell for auscultation of the lungs because it a. amplifies all types of sounds. b. filters extraneous sounds. c. pinpoints focal sound areas. d. transmits high-pitched sounds. e. transmits low-pitched sounds. ANS: D Unless specially modified, the stethoscope does not amplify sound, nor does it filter sound or pinpoint focal sounds. The stethoscope does transmit sound waves from the source to the ear. The diaphragm is the better source because it transmits the normally high-pitched sounds of the lung and has a broader area from which to listen. REF: p. 277 • Breath sounds normally auscultated over most of the lung fields are called a. vesicular. b. hyperresonance. c. bronchial. d. tubular. e. bronchovesicular. ANS: A The low-intensity sounds heard over most healthy lung tissue are called vesicular breath sounds. REF: p. 277 • Breath sounds normally heard over the trachea are called a. bronchovesicular. b. amphoric. c. crepitus. d. vesicular. e. bronchial. ANS: E The highest sounds in intensity and pitch are called the bronchial sounds, which are normally heard over the trachea. REF: p. 278 • When there is consolidation in the lung tissue, the breath sounds are louder and easier to hear, whereas healthy lung tissue produces softer sounds. This is because a. consolidation will echo in the chest. b. consolidation is a poor conductor of sound. c. air-filled lung sounds are from smaller spaces. d. air-filled lung tissue is an insulator of sound. e. consolidation causes hyperinflation of the lungs. ANS: D Whereas air is a poor conductor of sound, more dense consolidation promotes louder sounds and is a better conductor of sound. REF: p. 278 • The middle lobe of the right lung is best auscultated over the a. anterior chest. b. posterior chest. c. axilla. d. midclavicular line. e. scapula. ANS: C The sounds of the middle lobe of the right lung are best heard in the right axilla. REF: p. 262 • Your older clinic patient is being seen today as a follow-up for a 2-day history of pneumonia. The patient continues to have a productive cough, shortness of breath, and lethargy and has been spending most of the day lying in bed. You should begin the chest examination by a. percussing all lung fields. b. auscultating the lung bases. c. determining tactile fremitus. d. estimating diaphragmatic excursion. e. auscultating the apices. ANS: B Because the patient has consolidation and has been recumbent and fatigued, the most appropriate first step is to listen to the lung bases before the patient gets exhausted. The lung bases would be the most likely sites for adventitious sounds. REF: p. 277 • Your trauma patient has no auscultated breath sounds in the right lung field. You can hear adequate sounds in the left side. A likely cause of this abnormality could be that the patient a. has a closed head injury. b. has minimal fluid in the pleural space. c. is moaning and in severe pain. d. is receiving high oxygen flow. e. has a pneumothorax. ANS: E Trauma to the chest can cause an exudative pleural effusion or pneumothorax. In the affected areas, the breath sounds are diminished to absent. REF: p. 285 • Adventitious breath sounds previously referred to as rales has been replaced with the term a. wheezes. b. crunches. c. vesicular. d. crackles. e. rhonchi. ANS: D The term rales has been replaced with the term crackles to describe the sound more precisely. REF: p. 279 • To distinguish crackles from rhonchi, you should auscultate the lungs a. before and after the patient coughs. b. first at the lung base and then at the apex. c. with the patient inhaling and then exhaling. d. with the patient prone and then supine. e. with the patient recumbent and then sitting. ANS: A To distinguish between crackles and rhonchi, ask the patient to cough and auscultate again over the same area. Rhonchi, because they represent secretions in larger airways, can clear with coughing. REF: p. 279 • A musical squeaking noise heard on auscultation of the lungs is called a. stridor. b. rales. c. rhonchi. d. wheezing. e. friction rub. ANS: D Wheezes are continuous, high-pitched musical sounds that can be heard on inspiration and expiration. REF: p. 280 • To distinguish between a respiratory friction rub and a cardiac friction rub, ask the patient to a. hold his or her breath. b. lean forward. c. say “99” while you palpate the anterior chest. d. identify the location of his or her pain. e. arch backward. ANS: A A respiratory friction rub results from inflamed pleura rubbing against each other during the respiratory cycle, so if the breath is held, the rub stops. REF: p. 280 • In what position can the mediastinal crunch (Hamman sign) be heard best? a. In a supine position b. Lying on the left side c. Sitting completely upright d. With the head elevated 30 degrees e. In a prone position ANS: B The Hamman sign is heard with mediastinal emphysema. The adventitious breath sounds are synchronous with the heartbeat and are heard best when the patient leans to the left or lies down on the left side—these maneuvers bring the heart muscle closer to the chest wall. REF: p. 280 • Changes in clarity and volume of spoken sounds during auscultation of the lungs can help you distinguish a. crepitus from stridor. b. a foreign body from a purulent exudate. c. pulmonary edema from pleurisy. d. a right from left tracheal deviation. e. consolidation from airway constriction. ANS: E When chest auscultation results in decreased breath sounds or wheezes, the examiner can use techniques that involve the spoken word to distinguish these adventitious breath sounds as a result of consolidation rather than narrowing of a patent lumen. REF: p. 280 • During chest assessment, you note the patient’s voice quality while auscultating the lung fields. The voice sound is intensified, there is a nasal quality to the voice, and the e’s sound like a’s. This is indicative of a. lung consolidation. b. emphysema. c. bronchial obstruction. d. pneumothorax. e. asthma. ANS: A Vocal resonance, as described, indicates lung consolidation. Sounds are transmitted more clearly through consolidation rather than air. Conditions of air trapping such as emphysema and asthma would not produce vocal resonance sounds; bronchial obstruction would more likely result in a wheeze. Pneumothorax would result in diminished or no breath sounds. REF: p. 280 • During chest assessment, you note the patient’s voice quality while you are auscultating the lung fields. The voice sound is intensified, there is a nasal quality to the voice, and e’s sound like a’s. This sound described is called a. sonorous. b. bronchophony. c. pectoriloquy. d. egophony. e. resonance. ANS: D When the intensity of the spoken voice is increased, there is a nasal quality in which the e’s become stuffy broad a’s. This technique is called egophony. REF: p. 280 • How is the sputum of a viral infection different from the sputum of a bacterial infection? a. There is more sputum production with viral conditions than bacterial infections. b. The sputum is odorous with viral conditions and nonodorous with bacterial infections. c. The sputum is yellow, green, or rust colored with bacterial infections and mucoid with viral. d. The sputum is much thinner with bacterial infections and viscid with viral. e. Viral pneumonia sputum is never blood streaked. ANS: C The more likely differentiating characteristic between viral and bacterial sputum is the color. Whereas viral infections typically produce mucoid sputum, bacterial infections produce yellow, green, or rust-colored sputum. REF: p. 266 • The respiratory rate of a newborn infant is expected to range from _____ breaths/min. a. 10 to 20 b. 20 to 30 c. 40 to 60 d. 30 to 80 e. greater than 80 ANS: C The expected rate varies from 40 to 60 respirations per minute, although a rate of 80 is not uncommon REF: p. 281 • A signal for alarm during newborn chest assessment is a. crackles. b. rhonchi. c. gurgles from the gastrointestinal tract. d. stridor. e. a mobile xiphoid. ANS: D Crackles and rhonchi at birth are caused by the presence of remaining fetal fluid; intermittent gurgles are transmitted bowel sound through the thin-walled chest and are not alarming; stridor is alarming at any age. The newborn’s xiphoid process is more mobile and prominent than in older children. REF: p. 281 • Bronchovesicular breath sounds in young children that are loud and harsh are an indication of a. an accumulation of fluid. b. malignant tumors or solid masses. c. normal, thin chest wall structures. d. pus-filled abscesses and tumors. e. tension pneumothorax. ANS: C Young children’s chest walls are usually thin and therefore able to normally transmit loud, harsh, and more bronchial breath sounds than can adults. REF: p. 282 • The pregnant woman is expected to develop a. tachypnea and decreased tidal volume. b. deep breathing but not more frequent breathing. c. dyspnea and increased functional residual capacity. d. bradypnea and increased tidal volume. e. tachypnea and increased functional residual capacity. ANS: B In pregnant women, tidal volume and vital capacity increase, and functional residual capacity decreases. Also, pregnant women breathe more deeply but not more frequently. REF: p. 282 • Expected respiratory changes of normal aging include a. increased chest expansion. b. more frequent use of respiratory muscles. c. accentuated lumbar curve. d. more prominent bony structures. e. flattening of the dorsal thoracic curve. ANS: D In older adults, chest expansion is decreased, and there is less use of respiratory muscles because of muscle weakness. The dorsal curve of the thoracic spine is prominent with flattening of the lumbar curve with bony landmarks becoming more prominent because of loss of subcutaneous tissue. REF: p. 282 • Dullness to percussion in intercostal spaces is most consistent with the presence of a. asthma. b. empyema. c. pneumonia. d. sickle cell disease. e. pneumothorax. ANS: C The expected percussion tone over normal lung tissue, accessible in the intercostal spaces, is resonance. Dullness would indicate an area of consolidation, as is seen with pneumonia. REF: p. 274 • Which condition requires immediate emergency intervention? a. Patient with pleuritic pain without dyspnea b. Patient with fever and a productive cough c. Patient with tachypnea but no chest retractions d. Patient with pleuritic pain and rib tenderness e. Patient with absent breath sounds and dull percussion tones ANS: A A patient who experiences unexpected pleuritic pain without prior respiratory distress or dyspnea has most likely developed a pulmonary embolism, a condition with a high mortality rate. REF: p. 290 • A 29-year-old patient presents with a new complaint of productive cough with purulent sputum. He also complains of right lower quadrant abdominal pain. You suspect pneumonia in the _____ lobe. a. right lower b. right middle c. right upper d. left upper e. left lower ANS: A Right lower lobe pneumonia can stimulate the tenth and eleventh thoracic nerves, causing right lower quadrant pain, and simulate an abdominal process. REF: p. 288 • Epiglottitis has frequently associated with infection by which organism? a. Respiratory syncytial virus b. Haemophilus influenzae type B c. Adenovirus d. Parainfluenza virus e. Human metapneumovirus ANS: B Epiglottitis is an acute inflammation of the epiglottis caused by bacterial invasion. Immunization against the bacterium Haemophilus influenzae type B has greatly reduced the incidence in the United States. All of the other choices are viruses associated with bronchiolitis. REF: p. 291 [Show More]
Last updated: 1 year ago
Preview 1 out of 31 pages

Reviews( 0 )
Recommended For You
*NURSING> QUESTIONS & ANSWERS > NURS 612 exam 3CA: All Answers Explained By Instructor (All)

NURS 612 exam 3CA: All Answers Explained By Instructor
NURS 612 exam 3CA: All Answers Explained By Instructor • Conversion of fat-soluble wastes to water-soluble material for renal excretion is a function of the a. spleen. b. kidney. c. liver. d. panc...
By Slown , Uploaded: Nov 08, 2021
$8
Business> QUESTIONS & ANSWERS > CLM 031 EXAM (All)

CLM 031 EXAM
CLM 031 = 100% Question 1: 5b Select the statement that is correct concerning performance work statement (PWS) requirements: - All answers are correct. - PWS should describe requirements necessary...
By Book Worm, Certified , Uploaded: Nov 03, 2022
$5
*NURSING> QUESTIONS & ANSWERS > PHIL 347 Week 6 Checkpoint Quiz. Score 100/100 (All)

PHIL 347 Week 6 Checkpoint Quiz. Score 100/100
Question: What are the three fundamental reasoning strategies listed in the text? Question: What is comparative reasoning? On what skill is it based? Question: We learned four tests for evaluating...
By Amanda Rosales , Uploaded: Mar 24, 2021
$7
Business> QUESTIONS & ANSWERS > BUSINESS 1007 (All)

BUSINESS 1007
BUSINESS 1007 07 Key 1. (p. 178) Managers utilize organizational resources such as employees, information, and equipment to accomplish goals. 2. (p. 178) The main job of managers today is to w...
By Kirsch , Uploaded: Oct 19, 2019
$6
Anthropology> QUESTIONS & ANSWERS > KOR 352 FA19 101 week 8 Quiz. Already Graded A (All)

KOR 352 FA19 101 week 8 Quiz. Already Graded A
KOR 352 FA19 101: Week 8 Quiz Question 1 (0.25 points) Which of the following is not true of Kim and Finch’s observations during their field research in South Korea from 1997 to 2000? Question 1 o...
By Kirsch , Uploaded: Oct 17, 2019
$9
E-Commerce> QUESTIONS & ANSWERS > ESOC 316 Digital Commerce - University Of Arizona. Midterm Quiz. 20 Q&A. 100% Score (All)
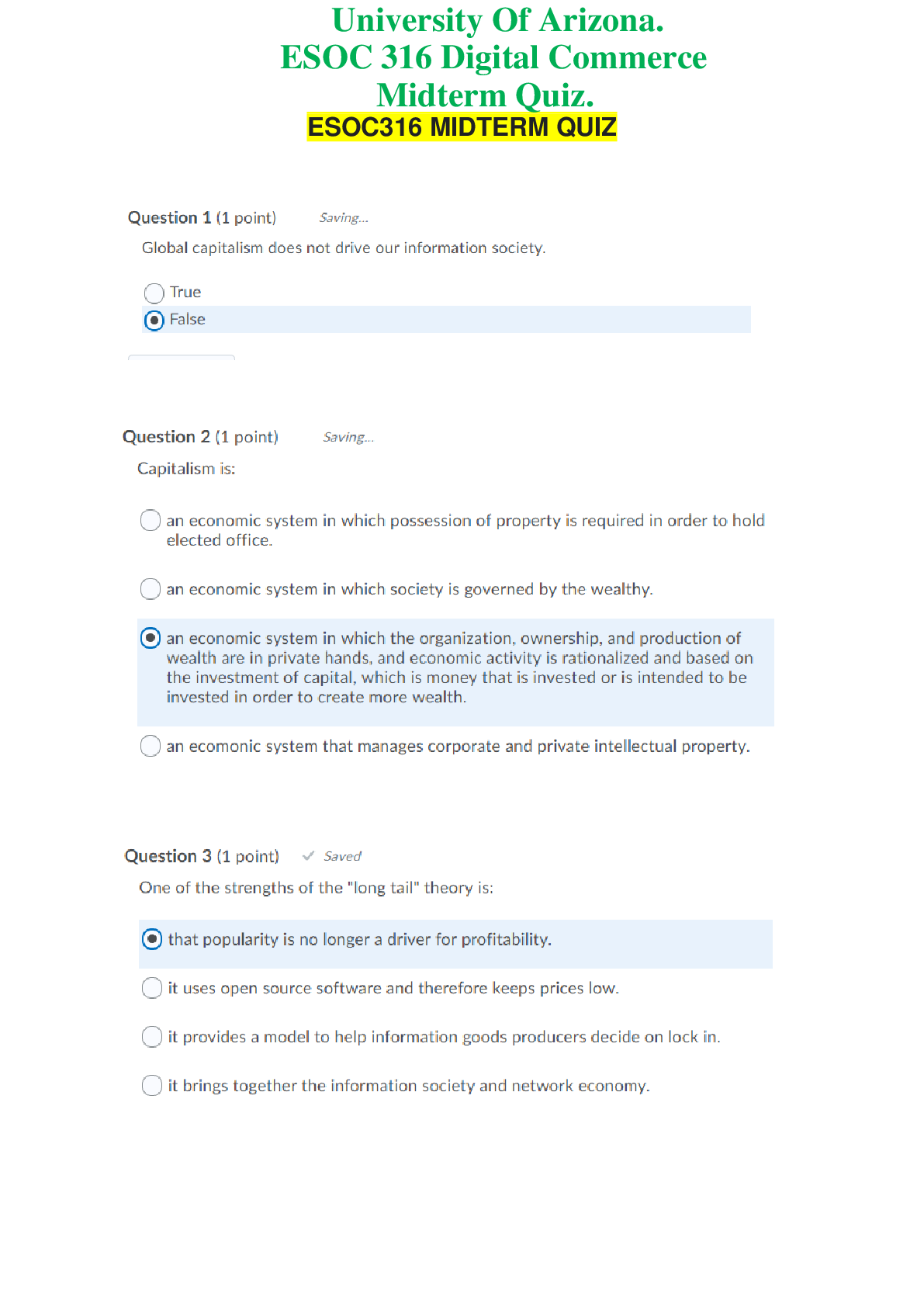
ESOC 316 Digital Commerce - University Of Arizona. Midterm Quiz. 20 Q&A. 100% Score
ESOC 316 Digital Commerce - University Of Arizona. Midterm Quiz. 20 Q&A. 100% Score ESOC316 MIDTERM QUIZQuestion 6 (1 point) Saved Information has several properties that make information goods...
By Kirsch , Uploaded: Oct 15, 2019
$9.5
Marketing> QUESTIONS & ANSWERS > Marketing Management Chapter 2 to Chapter 10 Q&A (All)

Marketing Management Chapter 2 to Chapter 10 Q&A
Chapter 2 to Chapter 10 Chapter 2: Developing Marketing Strategies and Plans GENERAL CONCEPT QUESTIONS Multiple Choice 66 Chapter 1: Marketing: Managing Profitable Customer Relationships...
By Kirsch , Uploaded: Oct 14, 2019
$10
Marketing> QUESTIONS & ANSWERS > MKT 530 Customer Relationship Management. 155 Questions and Answers (All)

MKT 530 Customer Relationship Management. 155 Questions and Answers
MKT 530 All Questions and Answers MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) As the manager of an organization that is att...
By Kirsch , Uploaded: Oct 14, 2019
$10
Art> QUESTIONS & ANSWERS > MAS 337 Exam 1. Graded A (All)

MAS 337 Exam 1. Graded A
MAS 337 Exam 1 Match the son with its corresponding region. 1.Oaxaca 2.Veracruz 3.Michoacan 4.Jalisco 5.Hidalgo 1. Son istemeno 2. Son Jarocho 3. Son Abajeno 4. Son Jalisciense 5. Son Huast...
By Kirsch , Uploaded: Oct 14, 2019
$6
Art> QUESTIONS & ANSWERS > MUS 337 Final Exam Graded 100%. (All)

MUS 337 Final Exam Graded 100%.
MUS 337 Final Daisy Moreno-Cota Fri Dec 11 12:59:42 PST 2015 Tone or aural color Volume and articulation of sounds Frequency of the tone Phonic structure or relationships between the sounds Dura...
By Kirsch , Uploaded: Oct 12, 2019
$9
Document information
Connected school, study & course
About the document
Uploaded On
Jul 12, 2019
Number of pages
31
Written in
Additional information
This document has been written for:
Uploaded
Jul 12, 2019
Downloads
0
Views
418






